Dr Elena Galkina – Immune Control of Initiation and Progression of Atherosclerosis
Atherosclerosis is a global health issue. Atherosclerosis is a multifactorial chronic inflammatory disease characterised by the accumulation of modified lipoproteins and immune cells in the aortic wall, vascular dysfunction, low-grade chronic inflammation, and formation of dangerous atherosclerotic plaques within the medium and large size vessels. Atherosclerosis is a prominent cause of cardiovascular diseases and mortality in many countries and this disease is closely associated with type 2 diabetes. Dr Elena Galkina, Professor of Microbiology and Molecular Cell Biology at Eastern Virginia Medical School, USA, has been working to determine the immune processes involved in an attempt to identify much-needed novel therapies.
The Immune Link with Atherosclerosis
A host of immune cell types have been associated with the initiation and progression of atherosclerosis. Dr Elena Galkina, Professor of Microbiology and Molecular Cell Biology at Eastern Virginia Medical School, USA, has identified the presence of many immune cell types, including both B- and T-lymphocytes, within normal aortic tissues as well as atherosclerotic tissue.
Furthermore, Dr Galkina has demonstrated that at least partial control of both T- and B-lymphocytes is managed by L-selectin, a molecule known to be involved in the ‘homing’ of T-cells to specific lymph nodes.
Function of B-lymphocytes in Atherosclerosis
Atherosclerosis, the leading cause of cardiovascular disease, accounted for approximately one-third of deaths in the USA in 2010. In an effort to reduce the rate of atherosclerosis development and progression, drugs or lifestyle changes are prescribed clinically. Unfortunately, this strategy only delivers an incomplete reduction of atherosclerosis.
Dr Galkina’s team indicate the imperative nature of further investigation into the pathways that may confer protection against initiation and progression of atherosclerosis. There is a substantial body of evidence that demonstrates the involvement of both the innate and adaptive immune response in the chronic inflammation that initiates and promotes atherosclerosis. Different cell types and even different sub-groups of the same cell type may be either pathological or protective with regards to atherosclerosis.
As the team has shown, B-cells are found in both atherosclerotic and normal aortic tissue, with differing ratios of B-lymphocytes of a specific sub-type being associated with atherosclerosis, both protective and disease-promoting.
It is largely accepted that B-cells do have a role in the initiation of atherosclerosis; however, the activation mechanism and the balance between protective versus disease promoting B-cell types remains to be elucidated.

Dr Elena Galkina and Colleagues
B-Cells and mLDL Uptake: Pathways and Cell Function Alterations
The research team is proposing to extend their work in the area of B-cell function and specific pathways for mLDL uptake, defining the pathways and, critically, the effect of this uptake on B-cell function. Initial research supports the induction of inhibitory pathways and changes in B-cell phenotype.
GRAIL and other E3 ligases are known to play a role in inducing tolerance in some immune cells, that is, they prevent the immune cell from responding to its own antigen target. Having demonstrated the presence of GRAIL and E3 ligases in B-cells, a collaborative team led by Dr Galkina and Dr Nurieva now proposes that a GRAIL-dependent mechanism is an inhibitory pathway that assists in regulating the B-cell activation threshold and induction of B-cells which do not respond to their antigen (anergic B-cells).
In their future plans, the team aims to identify the molecular mechanisms by which GRAIL exerts these effects on B-cells and the association with atherosclerosis.
Effector T-cells and Their Influence on Atherosclerosis Development
Dr Galkina and her colleagues have investigated the mechanism by which T-lymphocytes are involved in progressing atherosclerosis. Specifically, they interrogated the role of a receptor present on the surface of a sub-group of T-cells, CXCR6. They detected a significant correlation between this receptor expression on T-cells and atherosclerosis development.
In the absence of CXCR6, aortic lesion formation was found to be half that of CXCR6 sufficient mice. In addition, CXCR6 was positively associated with INF-γ, that is, where CXCR6 was low or absent, the concentration of pro-inflammatory cytokines was also reduced. Conversely, higher levels of CXCR6 induced production of INF-γ which, in turn, increased the recruitment of T-cells and macrophages (large white blood cells which are part of the immune system and a key component of atherogenesis) via up-regulation of a number of expressed proteins. Indeed, the team found that a population of CXCR6 deficient mice had a 90% reduction in one important sub-group of macrophages within the aorta.
Controlling Diabetes-associated Cardiovascular Disease
Cardiovascular disease related to atherosclerosis is increasing. Given the established link between inflammation of fat tissue, loss of beta cell function in the islets, and insulin resistance, the team of Dr Galkina and Dr Nadler team now intends to interrogate the link between loss of beta cell function and cardiovascular disease (CVD). They propose that identification of a shared pathway opens the door to developing dual-purpose therapies, that is, a methodology that addresses both beta cell decline and CVD.
Atherosclerosis is recognised as a major factor related to CVD in diabetic patients. As we have seen here, it is clear that atherosclerosis is a highly complex condition, involving a multitude of different pathways and systems throughout the body, and critically, includes the inflammatory immune response. Atherosclerosis-related inflammation is driven by a complex interaction and balance of immune cell subsets. However, within this myriad of immune cell interactions, there is a body of evidence that highlights the important role of myeloid cells in this damaging pathology.
Initiation of Atherosclerosis in Insulin Resistance
Investigating the link between atherosclerosis, obesity, insulin resistance, and type 2 diabetes, the research team of Dr Galkina and her EVMS collaborators Dr Nadler and Dr Dobrian established a link between STAT4, an immune regulatory factor, and increased inflammation in atherosclerosis and insulin resistance. Thereafter, Dr Galkina’s team focused their efforts on the effect of STAT4 on initiation of atherosclerosis, and specifically, the formation of plaques in cases of insulin resistance.
Using an animal model that displays both atherosclerosis and insulin resistance, the team found that low/no STAT4 levels leads to reduced atherosclerosis and enhances the metabolic response. Looking directly at the numbers of plaques in STAT4-deficient mice compared to diet-aligned controls, they found significantly fewer lesions – up to a 36% reduction. Furthermore, the plaque area at the aortic root was significantly smaller in the STAT4-deficient mice compared to controls.
The team extended the study timeline to account for the later stages of plaque formation and found that STAT4-deficient animals continued to show reduced plaque burden (at a rate of approximately 45% reduction) compared to matched controls.
Cellular Level Effects of STAT4 on Atherosclerosis Initiation
When the research team focused on the role of STAT4 with respect to immune cell infiltration and immune reactions, they found that the initiation of atherosclerosis was affected via pro-inflammatory macrophage activity, altering the ratio of two important sub-groups of T-lymphocytes, leading to local immune response modulation within the aortic cell wall in insulin resistance-accelerated atherosclerosis.
Importantly, these findings suggest a possible therapeutic role for the modulation of STAT4 expression in reducing the accelerated atherosclerosis that is associated with insulin resistance and type 2 diabetes.
In their future work, Dr Galkina’s and Dr Nadler’s research groups plan to untangle the pathways that drive myeloid cell activation and differentiation in atherosclerosis. They have previously investigated the important role of STAT4 in the mouse model, and they have demonstrated that deficiency – or blocking – of this important molecule conveys protection against atherosclerosis. They found that this occurs via control of macrophage activation and disruption of the delicate balance of cell recruitment, death, and proliferation. These areas of cellular activity are vital to the progress of their work.
The team will extend the reach of their work by investigating the role of STAT4 activation of neutrophils, which is known to lead to beta cell dysfunction, decreased metabolic activity, and increased atherosclerosis. The team hypothesises that there is a common pathway, linked to STAT4, which targets macrophages and neutrophils to progress the dual pathologies of type 2 diabetes and atherosclerosis. Importantly, this research will inform the development of innovative treatments to maintain beta cell mass and simultaneously reduce the accelerated cardiovascular disease which is strongly correlated with pre-diabetes and diabetes.
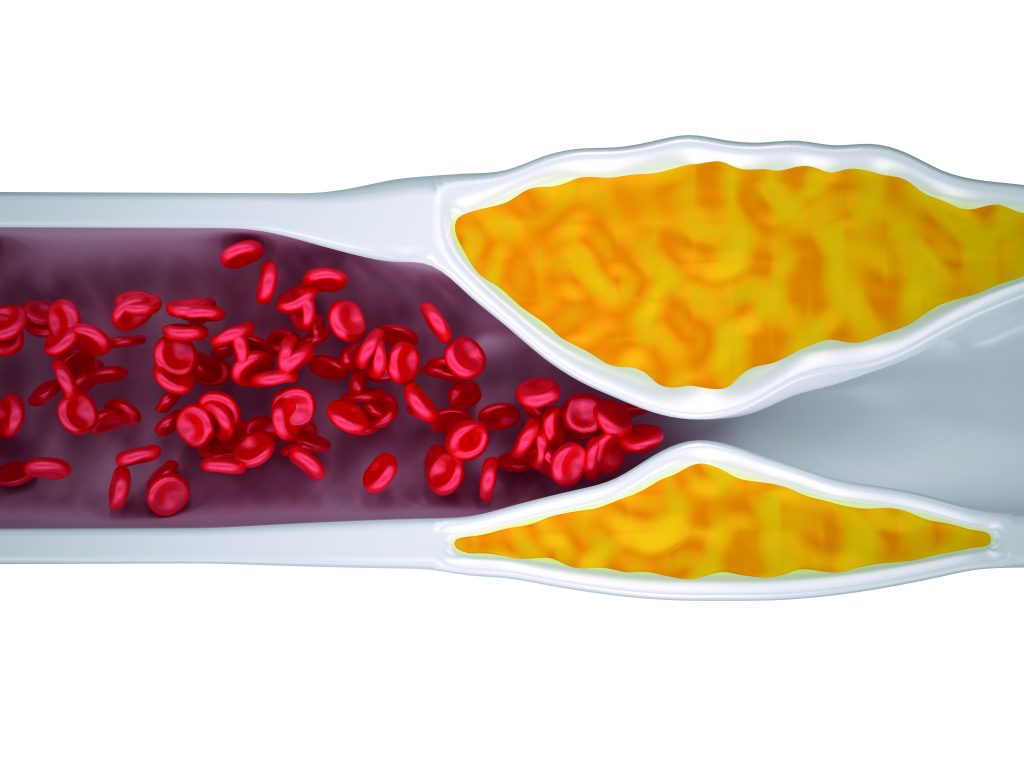
Diagram of Atherosclerosis: A Clogged Artery
Lymphocyte Populations and Pro-inflammatory Cytokines in Islet functions
It is well established that metabolic stress from excessive nutrition provokes islet inflammation and dysfunctions via lipotoxicity, and oxidative and endoplasmic reticulum stress, resulting in type 2 diabetes. While the role of the immune system in adipose tissue inflammation in type 2 diabetes is becoming more and more clear, very little is known about the impact of the immune system on islet health and functions in the conditions of type 2 diabetes. Thus, Dr Galkina and Dr Imai, an endocrinologist at the University of Iowa, initiated a project to determine lymphocyte and cytokine profiles in islets from normal human donors and type 2 diabetics. They found higher levels of CCL2, a protein that recruits specific immune cells to a site of inflammation, and TFN-α, an inflammatory cytokine, in type 2 diabetic derived islets when compared to normal islets.
In moderately functioning type 2 diabetic islets, some specific types of immune cells were increased in number when compared with poorly functioning islets. A range of both T- and B-lymphocytes was found in both healthy and damaged tissue; however, the team notes that the ratio of B-cells was significantly increased in the type 2 diabetic derived islets. The altered cell ratios point to a role of the adaptive immune response in islet damage. In terms of future plans, Dr Galkina and Dr Imai will focus their efforts on the characterisation of B lymphocyte functions in the regulation of islet dysfunction in pre-diabetic and type 2 diabetic patients.
Reference
https://doi.org/10.33548/SCIENTIA396
Meet the Team

Dr Elena V Galkina
Professor of Department of Microbiology and Molecular Cell Biology
Eastern Virginia Medical School
Norfolk, VA
USA
Dr Elena Galkina received her PhD in 1999 from the Saint-Petersburg Institute for Experimental Medicine, Russia. After completing a post-doctoral fellowship with the National Institute of Medical Research in the UK, she made the move to the University of Virginia, where she completed a postdoctoral fellowship before undertaking a series of academic position cumulating in her attainment of professorship in 2018. The focus of Dr Galkina’s research is the role of the immune system in cardiovascular disease, and in particular, on improving the understanding of immune cell involvement and efficacy of therapeutic agents with a view to reducing mortality. As a fellow of the American Heart Association, Dr Galkina is frequently invited to share her expertise at cardiovascular disease conferences and seminars, attended by international audiences.
CONTACT
W: https://www.evms.edu/directory/profiles/elena-v-galkina.php
KEY COLLABORATORS
Dr Jerry Nadler, New York Medical College, Valhalla, USA
Dr Mark Kaplan, Indiana University, Indianapolis, USA
Dr Roza Nurieva, MD Anderson Cancer Center, University of Texas, Houston, USA
Dr Larry Sanford, Eastern Virginia Medical School, Norfolk, USA
Dr Yumi Imai, University of Iowa, Iowa City, USA
Dr John Cambier, University of Colorado, Boulder, USA
Dr Anca Dobrian, Eastern Virginia Medical School, Norfolk, USA
FUNDING
NIH National Heart, Lung, and Blood Institute (NHLBI R01 HL139000 and NHLBI R01 HL142129)
American Heart Association (AHA AIREA33960546)
FURTHER READING
E Galkina, A Kadl, J Sanders, D Varughese, I Sarembock, K Ley, Constitutive lymphocyte recruitment into the aortic wall prior to development of atherosclerosis is partially L-selectin-dependent, Journal of Experimental Medicine, 2006, 203, 1273–82.
E Galkina, B Harry, A Ludwig, E Liehn, C Weber, K Ley, CXCR6 promotes atherosclerosis by supporting T cell homing, interferon gamma production and macrophage accumulation in the aortic wall, Circulation, 2007, 116, 1801–11.
MJ Butcher, D Hallinger, E Garcia, Y Machida, S Chakrabarti, J Nadler, EV Galkina, Y Imai, Association of proinflammatory cytokines and islet resident leucocytes with islet dysfunction in type 2 diabetes, Diabetologia, 2014, 57, 491–501.
P Taghavie-Moghadam, T Wassem, L Glenn, A Dobrian, M Kaplan, Y Yang, R Nurieva, J Nadler, E Galkina, STAT4 regulates CD8+Treg/Tfh cell axis and promotes atherogenesis in insulin-resistant Ldlr-/- mice, Journal of Immunology, 2017, 199, 3453–3465.

Creative Commons Licence
(CC BY 4.0)
This work is licensed under a Creative Commons Attribution 4.0 International License. 
What does this mean?
Share: You can copy and redistribute the material in any medium or format
Adapt: You can change, and build upon the material for any purpose, even commercially.
Credit: You must give appropriate credit, provide a link to the license, and indicate if changes were made.
More articles you may like
Stroke: A Global Challenge in Need of Innovation
Stroke is the third leading cause of both death and disability worldwide, but unfortunately, current diagnostic tools are unsatisfactory. Dr Roustem Miftahof and Dr Alexander Hermann at Advanced Biosimulation Technologies LLC, USA, are overcoming the limitations of existing diagnostic tools with the development of the Neuro-Glia-Vascular Unit Engine. This transformative tool for clinicians and biomedical researchers provides patient-specific health insights with the potential to improve care not only in stroke but across a range of neurological disorders.
Dr Shigetaka Hayano | The Rubber Revolution: Cracking the Code for Tire Recycling!
Traditionally, rubber waste was nearly impossible to recycle due to crosslinked sulphur bonds. But a team of researchers led by Dr Shigetaka Hayano from Zeon Corporation, in Japan, have achieved a groundbreaking feat in rubber recycling. Using mild conditions for the reaction, scientists have overcome the unfavourable cross-linked structure and have achieved recovery of rubber’s original monomers. This process restores cyclopentene monomers with 90% efficiency, allowing old tires and industrial rubber waste to be chemically recycled into high quality materials. If scaled up, this innovation could revolutionise waste management, reduce environmental pollution, and enable a circular economy for rubber production.
Prof Doron Lancet | Reproducing lipid micelles permit early Darwinian evolution
The origin of life has puzzled science and philosophy for thousands of years. While the prevailing scientific narrative is of an ‘RNA world’ or ‘polymers first’ approach, Prof Doron Lancet’s group of the Weizmann Institute of Science in Rehovot, Israel, present an alternative, describing a ‘lipid world’ scenario as a plausible origin for life, in which lipid micelles (simpler structures than cell-like vesicles) could have been nanoscopic protocell precursors. Core to the theory is that these micelles could exhibit catalysis and compositional self-reproduction, passing information through the mixture of their lipid components rather than through a genetic sequence.
Dr Sebastian Rabien | Making Membrane Mirrors for Future Space Telescopes
Mirrors play a key role in space telescopes, but to keep increasing the scale of this technology, mirrors need to be light and compact, so they can be transported in spacecraft, but also able to be adaptively corrected and controlled to ensure their accuracy. Dr Rabien and his colleagues from the Max Planck Institute for Extraterrestrial Physics, in Germany, have developed a technique to make extremely thin and lightweight mirrors, which can then be controlled with adaptive optics, making them a potential solution for larger space telescopes.




