Dr Arun Swaminathan – Improving the Diagnosis and Treatment of Neurological Diseases
Medical conditions that affect the brain can have severe impacts on people’s lives. Many of these conditions can be difficult to treat, including epilepsy which affects the brain to cause seizures and the common form of dementia known as Alzheimer’s disease. Dr Arun Swaminathan at the University of Nebraska Medical Center specialises in the treatment of epilepsy. He also collaborates with fellow researchers to explore treatment options for Alzheimer’s disease.
Finding the Best Treatments for Epilepsy
Across the globe, approximately 50 million people suffer from epilepsy. The majority of people who are diagnosed are prescribed anti-seizure medication to prevent seizures from occurring. However, a large number (about 25–30% of patients) are unresponsive to the treatment and require surgery. The surgery involves removing small parts of the brain that are thought to influence the seizures. Surgery has variable outcomes and success is dependent on many factors. These include the affected area of the brain and its baseline function as well as the surgical technique used.
Dr Arun Swaminathan at the University of Nebraska Medical Center and his colleagues sought to evaluate the treatment outcomes of epilepsy patients up to 20 years post-surgery. The researchers used past patient data to compare patients who had received a scalp electroencephalogram (EEG) or intracranial EEG. An EEG is a test that records the electrical wave patterns of the brain and can indicate if the brain activity is abnormal. This can be performed by either placing metal disks on the scalp, known as scalp EEG, or by placing electrodes into the brain (intracranial). Once this has taken place, surgery is performed and the outcome can be assessed using the Engel Epilepsy Surgery Outcome Scale. This ranges from the classification of an individual as being free of disabling features, to having rare seizures, demonstrating some improvement or finally, no worthwhile improvement or worsening.
Dr Swaminathan and his team observed that epilepsy surgery has good long-term outcomes in most patients. Those who had a temporal region of the brain removed, which is involved in hearing and speech, had the best outcome with scalp EEG alone, provided they had concomitant testing supporting pure temporal epilepsy only. Additionally, they found that some patients could suffer from cognitive problems such as memory loss, as well as depression or psychosis if they had surgery on the frontal region of the brain that is involved with cognitive skills, albeit these were mild in most patients that had them. The researchers also observed that using intracranial EEG had similar efficacy in finding the seizure onset zones as taking scans or images of the brain prior to the surgery in many patients.
Importantly, epileptic episodes do not always present as convulsive seizures. Some seizures can go unnoticed without any obvious clinical signs. This is dangerous as it can lead to delayed treatment response and result in the death of a patient. Dr Swaminathan and his team evaluated the use of EEG to detect nonconvulsive seizures using past patient data to see if experts could diagnose patients correctly given their EEG results. They also evaluated the best way to arrange the electrodes or metal plates onto the head for accurate diagnosis, otherwise referred to as a montage. They showed that the EEG could differentiate between normal and seizure-like wave patterns effectively and that a limited montage could provide sufficient efficacy in certain situations, especially if there were time constraints.

Learning from Experience to Improve Patient Care
Most medical conditions can be diagnosed using standard testing and tell-tale symptoms. Yet not every individual will present the usual symptoms that are associated with signs of a disease. Clinicians can take note of this and publish case reports to spread awareness of uncommon symptoms of a disease that have been observed in individual patients.
Dr Swaminathan observed that a patient with a genetic condition known as spinocerebellar ataxia type 8 was having seizures. This inherited condition leads to problems with movement, balance and coordination. Dr Swaminathan’s patient was also suffering from weakness over one side of the body and brain malfunction. Although seizures are rare for somebody suffering from this condition, Dr Swaminathan concluded that it was causing nonconvulsive seizures which could be treated using anti-epileptic therapy. This treatment resulted in an improvement for the patient. Dr Swaminathan thus suggests that even if seizures are a rare occurrence in somebody with a condition that affects the brain, patients should still see an epilepsy expert to speed up diagnosis and treatment for seizures.
Dr Swaminathan has also drawn from his experience observing patients to propose a novel way to diagnose cancer of the larynx or ‘voice box’. He identified that a 59-year-old patient was suffering from autoimmune encephalitis. This condition occurs when the body’s immune system, responsible for fighting infections and unhealthy cells, attacks healthy brain cells instead.
The patient was treated with anti-epileptic drugs and steroids to prevent seizures and reduce the activity of the immune system. Although the patient recovered, they returned to hospital a year later and was found to have a cancerous tumour on the larynx. The only indicator of this was high levels of striational antibodies which attack the proteins that make up muscle. Dr Swaminathan suggested that the cancer had caused the autoimmune condition and that although rare, the presence of striational antibodies could be used to diagnose this condition in other patients with similar presentations as well.
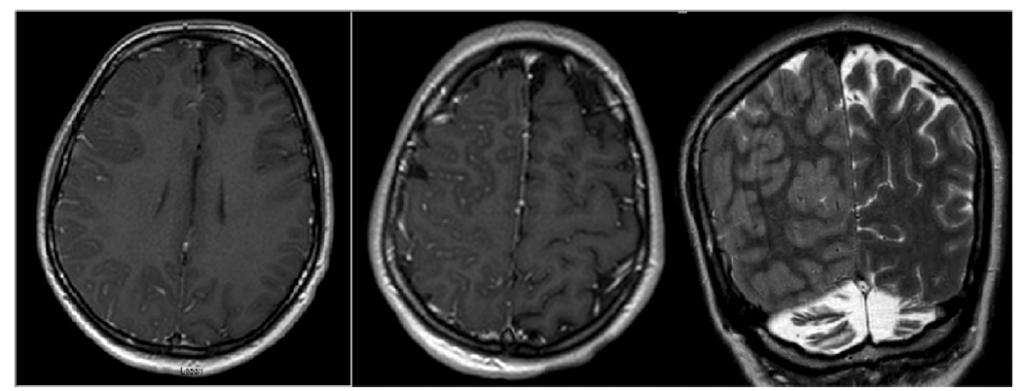
Magnetic resonance imaging scans in spinocerebellar ataxia type 8. Reproduced from A Swaminathan, Epilepsy in spinocerebellar ataxia type 8: a case report, Journal of Medical Case Reports, 2019, 13, 333.
A Novel Treatment for Epilepsy?
In many countries, cannabis is an illegal drug. However, in recent years it has been legalised to treat medical conditions including refractory epilepsy. Refractory epilepsy is a severe form of epilepsy that does not respond to recommended treatments. Cannabidiol (or CBD oil) is a chemical that is extracted from the cannabis plant and has been approved by the US Food and Drug Administration to treat epilepsy and prevent seizures in patients with refractory epilepsy syndromes like Lennox Gastaut Syndrome or Dravet’s Syndrome.
Dr Swaminathan and his colleagues used EEG and graphs to measure changes in brain network dynamics when patients with previously untreatable epilepsy are administered CBD. Brain network dynamics describe how parts of the brain connect and interact with one another and how this leads to changes in brain activity. Dr Swaminathan and his fellow researchers showed that treatment with CBD led to changes in brain network dynamics that could reduce seizures and that some of these brain network signals could predict which patients would be more likely to respond to CBD treatment. This opens up a new avenue to promote exploration of CBD as a treatment option for epilepsy in patients who have been previously difficult to treat.

Food for Thought
Further surprising treatment options have been proposed to treat epilepsy. Since the 1930s, it has been suggested that a ketogenic diet can prevent seizures in children and teenagers who suffer from refractory epilepsy. A ketogenic diet is a low carbohydrate, high fat diet which has become a trendy way to lose weight, but the exact mechanism of how this may prevent seizures is unknown.
Dr Swaminathan and his fellow researchers reviewed four different diet therapies and their effects on young patients from previous research. They concluded that there is no superior ketogenic diet that can be used to treat seizures in young patients but that some patients do respond better than others. They also pointed to the importance of maintaining a balanced diet for long-term health.
Other conditions that affect the brain may also be treated using a nutritional approach. Alzheimer’s disease is a form of dementia leading to irreversible memory loss and impairments to cognition that eventually reduce the patient’s quality of life and ability to self-care. Although it affects a large number of individuals, there is no known cure.
Nutritional approaches to slow, prevent or stop the progression of Alzheimer’s disease have been investigated. Dr Swaminathan and colleagues reviewed several of these approaches including the use of vitamins, antioxidants, plant flavonoids and omega-3 fatty acids. Despite being a safe treatment option, unfortunately, there is no overwhelming evidence that any of these approaches can reverse the effects of the disease. More optimistically, Dr Swaminathan suggests that nutritional interventions may still be able to supplement other approaches and improve treatment outcome along with improving the probability of preventing such diseases.
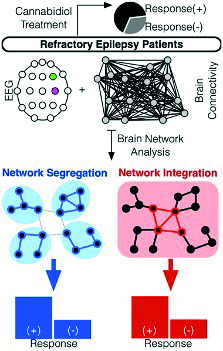
Reproduced from DE Anderson, D Madhavan, A Swaminathan, Global brain network dynamics predict therapeutic responsiveness to cannabidiol treatment for refractory epilepsy, Brain Communications, 2020, fcaa140.
Using Artificial Intelligence for Diagnostics
Not only is Alzheimer’s disease difficult to treat, but it is also hard to diagnose. Numerous methods have been proposed as potential diagnostic tests, including scanning the brain and assessing performance on psychological measures. Unfortunately, these methods can be imprecise or limited, prompting Dr Swaminathan and colleagues to seek out the use of novel technology to improve diagnostic approaches.
Artificial intelligence (AI) involves teaching computers to think and work like humans and comes with numerous applications. Dr Swaminathan and his collaborators used a branch of AI known as ‘deep learning’ to train a computer model to be able to classify whether a patient has Alzheimer’s using brain images taken by an MRI scan. They then tested the computer model with patient data and found that the model could accurately diagnose Alzheimer’s disease. Critically, further investigation could lead to this being used within clinical settings and to study other kinds of dementia and neurodegenerative disease as well.
As we can see, Dr Swaminathan’s clinical and research work extends beyond the field of epilepsy to improve the diagnosis, treatment, and ultimately, quality of life for patients with a broad range of neurological diseases.
Reference
https://doi.org/10.33548/SCIENTIA608
Meet the researcher

Dr Arun Swaminathan
University of Nebraska Medical Center
Omaha, NE
USA
Dr Arun Swaminathan is an Assistant Professor at the University of Nebraska Medical Center. He gained his medical degree from Lokmanya Tilak Medical College in Mumbai in 2004. He then moved to the USA to undertake a residency in neurology. Before commencing his current role, Dr Swaminathan undertook a clinical neurophysiology and epilepsy fellowship at the University of Pennsylvania. He now specialises in the treatment of epilepsy and works at a level 4 centre, which offers the highest level of epilepsy care for all patients. Dr Swaminathan is involved in aspects of epilepsy care, including diagnostics, treatment and epilepsy surgery. He is also involved in the field of research and has collaborated extensively with fellow researchers to explore treatment and diagnosis of epilepsy and Alzheimer’s disease. He hopes that his research can be implemented to improve the lives of patients with these diseases.
CONTACT
W: https://www.unmc.edu/neurologicalsciences/about/faculty/swaminathan.html
KEY COLLABORATORS
David Anderson PhD, University of Nebraska Medical Center
Vijaya Kolachalama PhD, Boston University
Olha Taraschenko MD PhD, University of Nebraska Medical Center
Deepak Madhavan MD MBA, Boys Town Hospital
FURTHER READING
S Qiu, PS Joshi, MI Miller, et al., Development and validation of an interpretable deep learning framework for Alzheimer’s disease classification, Brain, 2020, 143, 1920–1933.
A Swaminathan, Striational Muscle Antibody Positivity Heralding a Diagnosis of Autoimmune Encephalitis associated with Epiglottic Squamous Cell Carcinoma: A Case Report, Global Journal of Medical Research, 2020, 20, 8-F.
J Wells, A Swaminathan, J Paseka, C Hanson, Efficacy and Safety of a Ketogenic Diet in Children and Adolescents with Refractory Epilepsy-A Review, Nutrients, 2020, 12(6), 1809.
N Swingle, A Vuppala, P Datta et al., Olga Limited-Montage EEG as a Tool for the Detection of Nonconvulsive Seizures, Journal of Clinical Neurophysiology, 2020, doi:10.1097/WNP.0000000000000742.
DE Anderson, D Madhavan, A Swaminathan, Global brain network dynamics predict therapeutic responsiveness to cannabidiol treatment for refractory epilepsy, Brain Communications, 2020, fcaa140.
A Swaminathan, Epilepsy in spinocerebellar ataxia type 8: a case report, Journal of Medical Case Reports, 2019, 13, 333.
A Swaminathan, GA Jicha, Nutrition and prevention of Alzheimer’s dementia, Frontiers in Aging Neuroscience, 2014, 6, 282.

Want to republish our articles?
We encourage all formats of sharing and republishing of our articles. Whether you want to host on your website, publication or blog, we welcome this. Find out more
Creative Commons Licence
(CC BY 4.0)
This work is licensed under a Creative Commons Attribution 4.0 International License. 
What does this mean?
Share: You can copy and redistribute the material in any medium or format
Adapt: You can change, and build upon the material for any purpose, even commercially.
Credit: You must give appropriate credit, provide a link to the license, and indicate if changes were made.
More articles you may like
Stroke: A Global Challenge in Need of Innovation
Stroke is the third leading cause of both death and disability worldwide, but unfortunately, current diagnostic tools are unsatisfactory. Dr Roustem Miftahof and Dr Alexander Hermann at Advanced Biosimulation Technologies LLC, USA, are overcoming the limitations of existing diagnostic tools with the development of the Neuro-Glia-Vascular Unit Engine. This transformative tool for clinicians and biomedical researchers provides patient-specific health insights with the potential to improve care not only in stroke but across a range of neurological disorders.
Dr Shigetaka Hayano | The Rubber Revolution: Cracking the Code for Tire Recycling!
Traditionally, rubber waste was nearly impossible to recycle due to crosslinked sulphur bonds. But a team of researchers led by Dr Shigetaka Hayano from Zeon Corporation, in Japan, have achieved a groundbreaking feat in rubber recycling. Using mild conditions for the reaction, scientists have overcome the unfavourable cross-linked structure and have achieved recovery of rubber’s original monomers. This process restores cyclopentene monomers with 90% efficiency, allowing old tires and industrial rubber waste to be chemically recycled into high quality materials. If scaled up, this innovation could revolutionise waste management, reduce environmental pollution, and enable a circular economy for rubber production.
Prof Doron Lancet | Reproducing lipid micelles permit early Darwinian evolution
The origin of life has puzzled science and philosophy for thousands of years. While the prevailing scientific narrative is of an ‘RNA world’ or ‘polymers first’ approach, Prof Doron Lancet’s group of the Weizmann Institute of Science in Rehovot, Israel, present an alternative, describing a ‘lipid world’ scenario as a plausible origin for life, in which lipid micelles (simpler structures than cell-like vesicles) could have been nanoscopic protocell precursors. Core to the theory is that these micelles could exhibit catalysis and compositional self-reproduction, passing information through the mixture of their lipid components rather than through a genetic sequence.
Dr Sebastian Rabien | Making Membrane Mirrors for Future Space Telescopes
Mirrors play a key role in space telescopes, but to keep increasing the scale of this technology, mirrors need to be light and compact, so they can be transported in spacecraft, but also able to be adaptively corrected and controlled to ensure their accuracy. Dr Rabien and his colleagues from the Max Planck Institute for Extraterrestrial Physics, in Germany, have developed a technique to make extremely thin and lightweight mirrors, which can then be controlled with adaptive optics, making them a potential solution for larger space telescopes.




