Professor Mary Galea – Playing for Recovery
Improving recovery after nervous system injury has been Professor Mary Galea’s lifelong goal. Harnessing the power of video games, Professor Galea and her team at the University of Melbourne have developed the ‘Hand Hub’ to significantly enhance upper limb rehabilitation after stroke.
Freedom and control of movement forms a fundamental part of our daily lives. Loss of voluntary control of muscle movement can occur as a result of damage to the brain or the neurones that project from the brain, through the spinal cord, to the muscles controlling the arms and hands. In stroke this is caused by disruption of the blood supply to the brain, leading to damage and death of neurones in the affected area. Often this occurs in regions of the brain that initiate and control voluntary movement. Although brain tissue and nerves cannot regrow, the brain is a dynamic organ with the capacity to reorganise itself to allow motor function to recover following injury.
Stroke is a major cause of disability worldwide, affecting 5 million survivors who are left permanently disabled. The persistent loss of voluntary movement that occurs after stroke has a significant effect on quality of life. It affects people’s work and social life and has an impact on their psychological well-being, as well as placing an additional strain on carers and support agencies. During rehabilitation, much emphasis is placed on the function of lower limbs and finding ways to enable patients to walk again. However, a large number of day to day tasks important in our lives, require accurate control of hands and arms: from eating, to dressing yourself, to opening the front door with a key. Perhaps as a result of this, patients report that the loss of movement in their arms, is as important to them as loss of function in their lower limbs.
Professor Mary Galea of the University of Melbourne, Royal Melbourne Hospital, trained first as a clinical physiotherapist and has worked to rehabilitate survivors of stroke, traumatic brain injury, spinal cord injury, and other neurological conditions. She then went on to study neuroscience, and during her PhD she focused on the factors that promote recovery of the nervous system after injury. However, she reflects that she went on to develop ‘a special interest in the recovery of arm and hand function.’

‘My whole career has been focused on recovery of function after brain injury. I have made this a priority in my research because I believe we can do better if we think laterally, and think of ways to provide patients with the opportunity to help themselves.’
Rebuilding the Brain
‘Despite the increase in knowledge about recovery after stroke, very little time is devoted to upper limb rehabilitation because it is not a priority in getting a patient ready for discharge from rehabilitation,’ Professor Galea explains. She believes this is because ‘there are low expectations regarding the potential for recovery.’
A large proportion of stroke survivors (around 30 to 60%) fail to recover the use of their arm and hand. Research in animals suggests that after a brain injury occurs, repeated use of paralysed limbs stimulates reorganisation of the undamaged cortical areas of the brain. Repetitive exercises specifically targeted to improve a particular task stimulate the neurones in the cortex to produce new connections in a process called synaptogenesis. This process underlies the recovery of motor function and the ability to make voluntary movements after a stroke. In humans, clinical evidence suggests that high intensity task-specific training leads to the best outcome in terms of recovery, compared to simple repetitive exercises.
‘Activity of the affected arm and hand, whether volitional or induced through electrical stimulation or robotic means, helps to preserve the muscles and nerves and to drive reorganisation of the nervous system to promote recovery,’ Professor Galea states. She also believes that despite advances in our understanding of what is required to induce recovery, the current provision of physiotherapy in Australia is not sufficient to drive the cortical rearrangement required for recovery of upper limb movement. Due to the lack of successful rehabilitation, fewer resources are being devoted to the upper limbs, and there is currently little opportunity after discharge to continue with rehabilitation, especially in remote communities. ‘I would like to change the low expectations of health professionals regarding recovery of upper limb function’ says Professor Galea. Indeed, her team have shown that with appropriate exercise opportunities significant recovery of arm and hand function is possible.
Addressing the Evidence–Practice Gap
In order to address this gap between clinical practice and our understanding of what’s needed to drive recovery, Professor Galea’s team have developed an upper-limb rehabilitation programme using new inexpensive computer based technology and tested its effectiveness in a real-world setting. Patients with a range of different symptoms at the busy, resource limited, rehabilitation centre at the Royal Melbourne Hospital were given access to a range of devices to create additional exercise opportunities to promote the recovery of arm and hand movement in a ‘Hand Hub’.
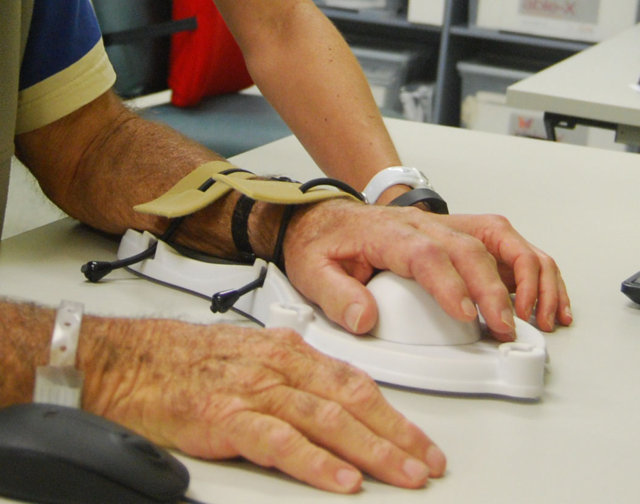
In this study, 92 patients, most of whom had suffered a stroke (and some with multiple sclerosis and loss of arm function due to tumours) underwent a six-week programme at the hospital where they visited the Hand Hub for an hour of arm and hand training at least three times a week for six weeks. The Hand Hub consists of three devices that patients can use, each getting progressively more difficult as movement improves or depending on the range of movement a patient has after injury. The first – the Able-M – is a table-top device for patients who struggle with very limited arm movements, which leads onto the Able-X, a light-weight handle-bar. Finally, the most challenging device is the ReJoyce station, which consists of a spring-loaded arm and involves practising tasks with daily household objects such as a doorknob, a key and two coin simulators.
Playing the Game
This equipment is run by game software that provides instant visual feedback on a patient’s progress, and allows them to move through different levels of difficulty. It also provides constant monitoring and information that the physiotherapist can use to assess progress. Up to five patients can use the equipment at once under the supervision of one physiotherapist and one health care assistant, increasing the number of people who can receive treatment quickly and cutting waiting times.
The games are interesting, challenging and fun, and therefore sustains the participants’ focus and motivation. The games have been designed so that after a while, patients stop thinking about the arm movement and focus on obtaining the goal of the games. This is thought to be a critical aspect of motor learning and encourages people to continue with the intensive exercise programme. After the six-week programme the participants showed significant improvements in their upper limb strength. This had a direct impact on their quality of life, improving their psychosocial well-being and cognitive abilities. Importantly, patients reported an increased ability to use their affected limb in everyday life, reducing the burden on carers.
This preliminary study revealed the potential of this novel approach. Now, Professor Galea’s team are now developing a tele-rehabilitation programme based on the positive results of the Hand Hub trial, to allow patient treatment to continue after discharge from hospital, in the comfort of their own homes.
Into the Future: Tele-rehabilitation
Access to rehabilitation services in the community is limited. During early rehabilitation, the number of arm movements made by patients to aid recovery is low compared to the hundreds of repetitions that have been shown to promote changes in cortical structure in animals. Tele-rehabilitation uses advances in robotics, sensors and game technology to dramatically increase the amount of treatment a patient receives. Patients in the preliminary Hand Hub study had to travel up to 550 km to reach the hospital for treatment. The fact that patients were willing to travel such a large distance was perhaps a reflection of the lack of resources in their local area, and how strongly people felt about recovering their hand function.
In order to help people in rural communities, the team have developed a system based on the same technology as that used in the hospital, which can be used at home and remotely monitored by a physiotherapist. Professor Galea’s aim is ‘to show that tele-rehabilitation is effective and to see it rolled out nationally, so that patients who currently cannot access rehabilitation for their affected upper limb, whether because of distance from rehabilitation services or lack of them, can benefit.’
A trial is currently underway with an increased number of patients in a rigorous randomised control trial to test the effectiveness of tele-rehabilitation with the Hand Hub and its cost effectiveness. Each participant in the trial has access to the Able-M and Able-X equipment at home, which are controlled by a set-top box through Wi-Fi, and can be connected up to any available TV or digital screen. Software is accessed through a cloud server, and therapists can remotely access performance and training records and guide people through on-line communication as their training progresses. The participants use the Hand Hub at home for an hour, every five days over eight weeks, and this is compared to a control group who have access to a web based game designed to enhance memory and attention. The control group is required in order to determine the effect of the Hand Hub exercises separate from the cognitive enhancement associated with playing the game.
Patients will be tested after eight weeks, six months and twelve months to observe long term changes. Evidence suggests that cortical rearrangement stimulated by such high intensity training can produce improvements that last for years. As confidence develops in using the affected limb, patients start to spontaneously use the affected arm or hand, leading to further improvements.
Access for Everyone
If the trial is successful it can be applied nationally in Australia and could be adopted in other countries across the world to enhance arm function recovery following stroke. The Hand Hub is already being adopted elsewhere in other rehabilitation units and in Australian communities by local stroke support groups.
This technology is adaptable and can be used to allow more cost and resource effective access to appropriate physiotherapy after different types of brain injury. Allowing everyone access to an enjoyable, motivating game that can improve quality of life, reducing the impact of loss of arm and hand function on the lives of the people affected and their carers. Professor Galea and her team would like to show how effective tele-rehabilitation can be, and to see it rolled out nationally and even internationally, so that stroke survivors everywhere can benefit, regardless of their location.
Meet the researcher

Professor Mary Galea
Department of Medicine
Royal Melbourne Hospital
University of Melbourne
Melbourne
Australia
Professor Mary Galea trained as a physiotherapist at the Lincoln Institute of Health Sciences and obtained a PhD in neuroscience at the University of Melbourne in 1992. She was then awarded a postdoctoral fellowship University of Melbourne, which led on to a senior lectureship and an appointment as Foundation Professor of Clinical Physiotherapy from 2001–2012. She was also the director of the Rehabilitation Sciences Research Centre at the University of Melbourne and Austin Health from 2004–2011. Currently, Professor Galea is a Professorial Fellow at the University of Melbourne in the Department of Medicine at the Royal Melbourne Hospital, where she carries out basic and clinical research into nervous system recovery after injury, with a focus on recovery of arm function. She has won numerous awards for her work including the Sir Winston Churchill Memorial Fellowship in 2007 and was inducted into the Victorian Honour Roll of Women in 2014.
CONTACT
E: m.galea@unimelb.edu.au
T: (+61) 3 8387 2017
W: http://bit.ly/MaryGalea
KEY COLLABORATORS
Professor Fary Khan, Director of Rehabilitation, Royal Melbourne Hospital
Dr Bhasker Amatya, Research Fellow, Royal Melbourne Hospital
Dr Eduardo Cofré Lizama, Research Fellow, Department of Medicine (Royal Melbourne Hospital), The University of Melbourne
Dr Andisheh Bastani, Research Fellow, Department of Medicine (Royal Melbourne Hospital), The University of Melbourne
Ms Marlena Klaic, Senior Occupational Therapist, Royal Melbourne Hospital
Dr Imogen Windle, Rehabilitation Registrar and PhD student, Royal Melbourne Hospital
Dr Arthur Hsueh, Health Economist, The University of Melbourne
Professor Leonid Churilov, Head of the Division of Statistics and Decision Analysis, Florey Neuroscience Institutes
FUNDING
Department of Medicine, University of Melbourne
REFERENCES
MP Galea, F Khan, B Amatya, A Elmalik, M Klaic, G Abbott, Implementation of a technology-assisted programme to intensify upper limb rehabilitation in neurologically impaired participants: A prospective study, Journal of Rehabilitation Medicine, 2016, 48, 522–528.