Dr Florence Bareyre – A Chordate with Destiny
Spinal cord injuries have garnered the dedication of countless researchers. Nevertheless, the path towards understanding and mastering neuronal repair in the central nervous system (CNS) remains more tortuous than even the tangled nerves themselves. It therefore seems apposite that Dr Florence Bareyre’s journey in neuroscience research began with one or two detours of its own.
Few phenomena outline human physiology’s limits more starkly and infamously than spinal cord injuries. Whether caused by local ischemia or inflammation, or the split-second result of trauma, a fully severed spinal cord is exceptional for its permanence, notorious for its evasion of successful treatments, and alarming in its implications for the remainder of a person’s life.
The spinal cord, a delicate bundle of neural cells and circuits, originates from the medulla oblongata in the brainstem and terminates near the top of the lumbar vertebral levels. It houses the neuronal circuitry involved in various reflexes, and links its companion in the CNS – the brain – to the peripheral nervous system (PNS). In its pivotal latter role, it serves as the envoy for signals from the brain to the muscles, and carries sensory signals in the opposite direction.
Its critical functions earn the spinal cord a reasonable degree of physical protection, including vertebral bone and three meningeal membranes that support the tubular structure and enclose it in adipose tissue and cerebrospinal fluid. Despite this protection, between 250,000 and 500,000 people suffer a spinal cord injury each year worldwide, and for many the prognosis is poor. Most spinal cord injury victims suffer lasting sensory or motor function loss and chronic pain, and many must live with paraplegia or quadriplegia and damage to the systems that regulate, for example, their bladder control, breathing or heart rate.
In contrast to the CNS, the PNS is known for its ability to regenerate and return function to damaged neurons. Researchers excitedly demonstrated in the 1980s that a permissive peripheral nerve graft could even allow certain mature CNS axons to regenerate. With the lack of intrinsic plasticity in the CNS taken as dogma, the subsequent discovery by Dr Florence Bareyre and colleagues that following partial lesions in the spinal cord axonal tracts could spontaneously sprout and restore function was spectacular.
‘In our laboratory, we are trying to understand the molecules important for axonal outgrowth, axonal guidance and synapse formation in order to design new therapeutic strategies to foster axonal remodelling and improve functional recovery after central nervous system injuries.’
Detour de Force
‘Since the beginning of my scientific training in 1996, I have always been attracted to understanding how nerve cells respond to CNS damage,’ says Dr Bareyre, who currently heads up her own laboratory at LudwigMaximilians Universität München, Germany, and has used her score of years in research to elucidate CNS remodelling mechanisms in some of the world’s most accomplished laboratories. Throughout her career, she has primarily used the rodent corticospinal tract (CST) to study how axonal connections rewire in response to injury.
She began her research career at University of Pennsylvania, investigating how therapeutic strategies limit neuronal cell death following experimental brain injury. Following a string of publications, she moved to Professor Martin Schwab’s laboratory at ETH Zurich to complete her PhD thesis. ‘To further understand how spontaneous recovery of function is achieved, I studied the reorganisation of the CST after spinal cord injury or inflammatory lesions. For this purpose, I combined advanced tracing techniques to follow the reorganisation
of hindlimb corticospinal connections on multiple anatomical levels.’
Dr Bareyre’s first great breakthrough arrived when she and co-workers at ETH Zurich definitively demonstrated that partial spinal cord lesions in mice can be bridged by socalled intraspinal ‘detour’ circuits, restoring the function of severed spinal cord pathways. The group showed that transected hindlimb CST axons sprouted neuronal offshoots, known as collaterals, that contacted functioning long propriospinal neurons rostrally to the site of the lesion. Dr Bareyre explains that they not only observed signs of plasticity in the spinal cord, but also found that the reorganisation of intraspinal connections was paralleled by remodelling of the cortical motor representation. Researchers had previously noted motor cortex reorganisation after neuronal damage, but these authors were rewarded for providing solid evidence for the basis of ‘detour’ circuit formation and its direct role in functional recovery and wider neurological impact with a place for their work in the prestigious journal Nature Neuroscience.
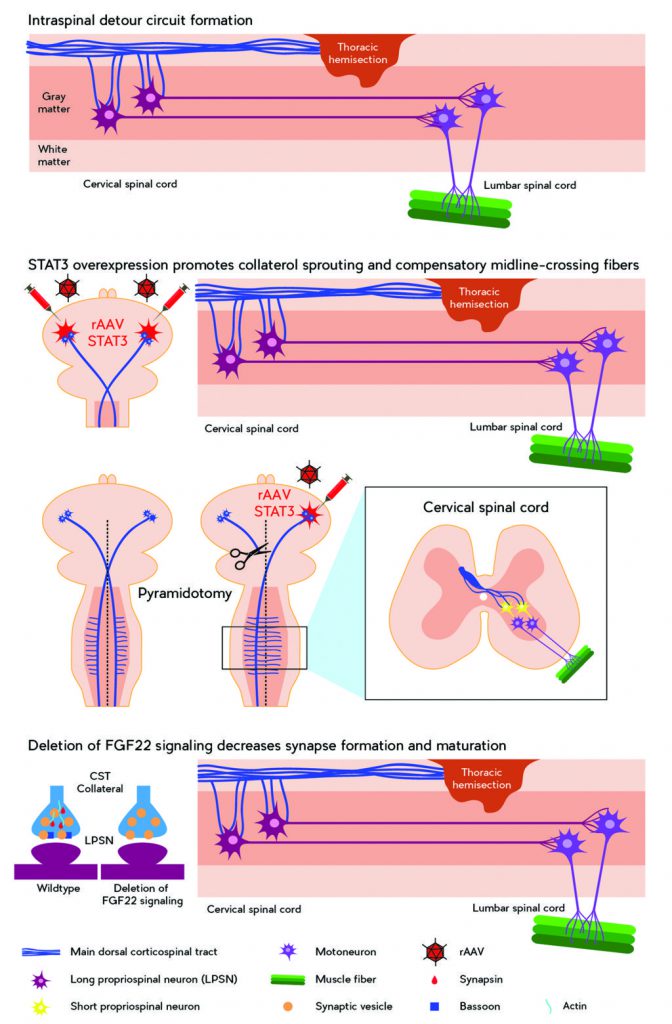
A follow-up study corroborated these findings in an animal model of multiple sclerosis. Rather than inducing traumatic lesions, the group instead targeted the CST with an inflammatory lesion that severely damaged the nerves. Despite the differing causes of the lesions, the findings were similar: local interneurons exhibited sprouting; CST axons above the lesion extended collaterals, forming a detour circuit; spared CST axons below the lesion increased their terminal branching; and the motor cortex was again remodelled.
‘The following important questions arose from these studies,’ recounts Dr Bareyre. ‘How do the growing axons find the appropriate path to their intraspinal targets and how do they form and stabilise synapses onto these targets?’ To gain insight into the principles that can regulate axonal pathfinding and synapse formation, Dr Bareyre joined the laboratory of Joshua Sanes at Harvard, one of the leading experts studying circuit formation in the developing nervous system.
Striking a Cord with Technicolour
At Harvard, Dr Bareyre bolstered her biological imaging toolkit by developing methods of visualising synapses using tagged peptides, a technique that proved very useful for monitoring synapse formation. She put this experience towards her next significant achievement, which she reported in Nature Medicine in 2005. In this work the authors gathered expertise in transgenic technology and generated a new transgenic mouse model in which the corticospinal tract is labelled with a fluorescent protein. Dr Bareyre envisioned that the CST-YFP mice would be useful for evaluating strategies designed to maximise remodelling and promote regeneration. To learn emerging in vivo imaging techniques that allow the direct visualisation of regrowing spinal axons and their path to the target cells in vivo, Dr Bareyre joined the Institute of Clinical Neuroimmunology at the LMU Munich.
Chasing the Peripheral Vision
There are clearly differences in the CNS and PNS that explain why the former lacks the latter’s knack for regrowth. Researchers have previously identified growth-inhibiting factors in the CNS and growthpromoting factors in the PNS. For example, particular proteins in CNS myelin and other molecules associated with astroglial scars are known to inhibit axon growth and plasticity. At the same time, the down-regulated expression of growth-promoting genes, which are highly expressed in damaged PNS neurons, also limits brain and spinal cord repair in the CNS. Contrasting the natural strategies adopted by the PNS and CNS after injury has therefore been a pivotal way for Dr Bareyre and other researchers to locate and exploit the factors involved in neuronal growth and plasticity. As you might expect, however, this is not a simple task.
In 2011, Dr Bareyre and colleagues employed in vivo time-lapse fluorescence microscopy, genetic modification and viral gene transfer to uncover the key molecular players in PNS plasticity that are lacking in the CNS. Lesions were introduced to the peripheral or central axon branches of the dorsal root ganglia, as they extend branches to both nervous systems. The group discovered that the transcription factor STAT3 plays a key role in initiating neuronal regeneration, with its absence limiting PNS outgrowth and overexpression greatly enhancing terminal branching and collateral sprouting after a CNS lesion.
Based on these promising findings, the group explored the potential of STAT3 in CNS plasticity further in 2013. They found that, although STAT3’s artificially sustained expression did enhance lesioned CST neuron sprouting, it unfortunately did not seem to influence the formation of intraspinal detour circuits. In a ground-breaking discovery, however, the group found that after a unilateral pyramidotomy (which interrupts the corticopsinal tract on one side of the body rostral to the pyramidal decussation), sustained STAT3 expression led to a 4- to 10fold increase in the number of collaterals crossing from the functioning side of the body to contact short propriospinal neurons and spinal motoneurons of the side affected by the unilateral pyramidotomy. Additionally, these connections led to some functional recovery, with cortical stimulation creating an EMG signal in the previously disconnected muscles – revealing the potential for extraordinary plasticity in the CNS.
Continuing Off the Beaten Pathways
Since this important observation, Dr Bareyre has enthusiastically continued her research into the processes underlying neuronal plasticity. For instance, her group at Ludwig-Maximilians Universität München also recently identified the first key regulator of synaptic formation in adults following injury: FGF22. Dr Bareyre found that the fibroblast growth factor FGF22 and its receptors are respectively expressed in spinal relay neurons and cortical projection neurons, and that blocking their expression hinders the functional recovery of mice with spinal cord injuries.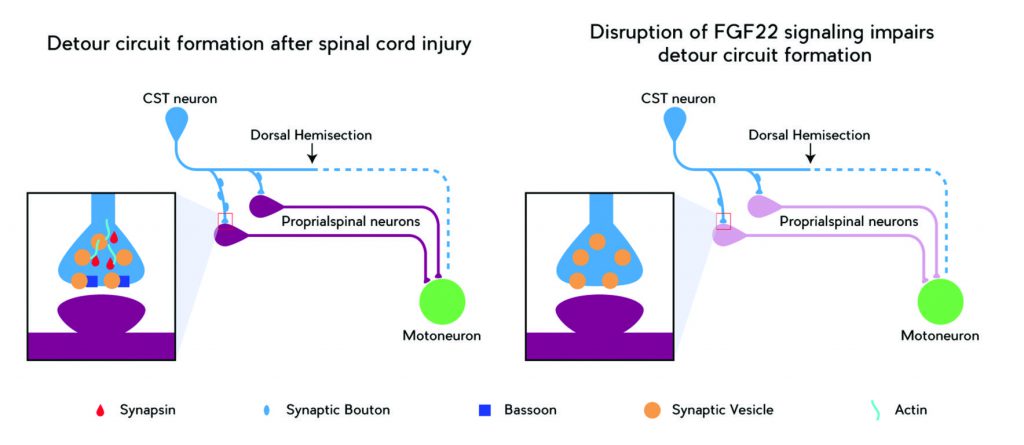
Dr Bareyre’s research group has been supported for 6 years by the German Federal Ministry for Research and Education, through a competitive national award aimed at supporting outstanding young female neuroscientists, 1 of 5 grantees over more than 70 applications. Her group is currently part of various research consortia funded by the German National Science Foundation and further supported by the wings for life spinal cord research foundation. Funding from these sources acts in much the same way as an action potential – it is the stimulus that triggers the group’s cascade of vital research activities and yields results far in excess of its face value. Some of the ongoing activities in Dr Bareyre’s laboratory include investigating the biochemical events underlying the improved outcomes during physical rehabilitation, and further delving into the nature of intraspinal detour circuits.
Dr Bareyre asserts that her laboratory will keep working along the previously described lines in order to keep discovering new molecules that are important for axonal remodelling following spinal cord injury. Lines of work currently followed by Dr Bareyre include, for example, investigating how overexpression of FGF22 can further promote postinjury axonal remodelling, understanding the how rehabilitation and voluntary training do impact functional recovery. ‘We then hope to be able to manipulate these molecules – also using combinatorial therapies – in order to improve functional recovery following spinal cord injury,’ she says.
The global scale of research into spinal cord injuries is reassuring, and important results and promising preclinical therapies are on the horizon due to Dr Bareyre’s group and others like it. Nonetheless, for those afflicted with CNS injuries, the next paradigm shift in spinal cord injury treatment surely cannot come soon enough. With luck, the label ‘permanent’ will soon acquire plasticity of its own.
Meet the researcher

Dr Florence Bareyre
Institute of Clinical Neuroimmunology
Hospital and Biomedical Center (BMC)
Ludwig-Maximilians Universität München
Munich, Germany
Dr Florence Bareyre obtained her PhD at the Brain Research Institute, ETH Zurich in 2003, after which she pursued postdoctoral research at Washington University, Harvard University and LMU Munich. She became a Group Leader at the Institute of Clinical Neuroimmunology, LMU Munich in 2008 and then also at the Biomedical Center, LMU Munich in 2015. She is a member of the Munich Centers for Neurosciences and a principal investigator in the Collaborative Research Center 870, the graduate school for neuroscience and the excellence cluster syNergy. Since 2014 she has served as a board member in the Collaborative Research Center 870. She has received several awards, among them the medal of excellence from the ETH Zürich, the SOBEK junior price for multiple sclerosis and an independent group leader award from the Federal Ministry of Education and Research. She studies spinal cord injuries and the mechanisms underlying the recovery process to develop new therapeutic strategies that can support spinal cord repair in neurological disease. She is married and has four children.
CONTACT
E: Florence.Bareyre@med.uni-muenchen.de
T: (+49) 89 2180 71663
W: http://www.klinikum.uni-muenchen.de/bareyre
KEY COLLABORATORS
Thomas Misgeld, TU Munich
Martin Kerschensteiner, LMU Munich
Klaus Conzelmann, LMU Munich
Hildegard Büning, University of Cologne
Doron Merkler, University of Geneva
Hisashi Umemori, Harvard University
FUNDING
German Federal Ministry for Research and Education
German National Science Foundation
Wings for Life Foundation
REFERENCES
A Jacobi, K Loy, AM Schmalz, M Hellsten, H Umemori, M Kerschensteiner, FM Bareyre, FGF22 signaling regulates synapse formation during post-injury remodeling of the spinal cord, EMBO J., 2015, 34, 1231–43.
C Lang, PM Bradley, A Jacobi, M Kerschensteiner, FM Bareyre, STAT3 promotes corticospinal remodelling and functional recovery after spinal cord injury, EMBO Rep., 2013, 14, 931–7.
FM Bareyre, N Garzorz, C Lang, T Misgeld, H Büning, M Kerschensteiner, In vivo imaging reveals a phase-specific role of STAT3 during central and peripheral nervous system axon regeneration, Proc Natl Acad Sci USA, 2011, 108, 6282–7.
FM Bareyre, M Kerschensteiner, T Misgeld, JR Sanes, Transgenic labeling of the corticospinal tract for monitoring axonal responses to spinal cord injury, Nat. Med., 2005, 11, 1355–60.
M Kerschensteiner, FM Bareyre, BS Buddeberg, D Merkler, C Stadelmann, W Brück, T Misgeld, ME Schwab, J. Exp. Med., 2004, 200, 1027–38.