Dr Tammy Movsas, MD, MPH – Towards a Brighter Future: How Zietchick Research Institute Plans to Transform Treatment for Retinal Disease
Both diabetic adults and premature babies are at risk for a similar type of eye disease that involves the growth of abnormal, blood vessels in the retina, the photosensitive layer of the eye. When this eye disease occurs in diabetics, it is called diabetic retinopathy and when it occurs in premature infants, it is called retinopathy of prematurity. The pathologic vessels, seen in both of these diseases, can pull on the retina and cause it to detach, leading to blindness. Dr Tammy Movsas (Executive Director and Principal Investigator) and Dr Arivalagan Muthusamy (Chief Scientist) at the Zietchick Research Institute, USA, are developing new therapeutics to treat these serious retinal diseases that affect both premature baby eyes and mature adult eyes, such as those of diabetic women.
Diabetic Retinopathy
Diabetes mellitus is a global problem and one that is increasing. Currently, approximately 5% of the global population is diagnosed as being diabetic. However, the World Health Organisation predicts that by the year 2030, we can expect there to be more than 360 million people afflicted by diabetes worldwide. Type 1 diabetes occurs when the body’s immune system attacks the pancreatic cells that are responsible for producing insulin and this is often diagnosed early in life. In contrast, type 2, the most common subtype of diabetes is often associated with obesity and typically onsets later in life. However, because of rising rates of obesity in youth, there has been a steep rise in the incidence of type 2 diabetes during the teenage and early adulthood years. In Type 2 diabetes, the body is either unable to produce enough insulin or becomes insensitive to the effects of insulin.

Diabetic retinopathy is the most common complication arising from diabetes, afflicting almost 35% of diabetic patients in developed countries. For diabetic women with retinopathy prior to pregnancy, there is a significant likelihood of their eye disease considerably worsening over the course of pregnancy. Due to the increasing number of young people with type 2 diabetes, there are more child-bearing aged women who are now affected by this. Despite the well-documented clinical awareness of this phenomenon, our knowledge regarding the underlying mechanisms of this exacerbation during pregnancy remains very limited.
Gonadotropins and the Eye
Dr Tammy Movsas (Executive Director and Principal Investigator) and Dr Arivalagan Muthusamy (Chief Scientist) at the Zietchick Research Institute (ZRI) are working with their colleagues to overcome the significant challenges posed worldwide by retinopathy. Their current work focuses on two related gonadotropin hormones. These are known as luteinising hormone (LH) and human chorionic gonadotropin (hCG). Both these hormones bind to the same receptor in the human body.
Gonadotropins are hormones that classically target reproductive organs such as the uterus and ovaries in females, and testes in males. For example, LH stimulates ovulation in teenage girls and women of childbearing age. Yet the importance of these hormones to the function of non-reproductive organs seems to be much greater than was first thought. On the basis of previously published research, Dr Movsas made the intriguing prediction that these hormones would also play a key role in retinal angiogenesis, that is, the development of new blood vessels in the eye.
Dr Movsas and colleagues were the first to demonstrate that a deficiency of LH receptors in the mouse eye negatively affects the vision enabled by the cone photoreceptors in the retina. Cone cells, named after their conical shape, are the retinal cells responsible for colour vision and for sharp central vision.
In an already landmark study, Dr Movsas and colleagues continued to show that LH is reliably present in the living human eye. In confirming their initial predictions, they also demonstrated that proliferative diabetic retinopathy is associated with increased levels of LH. In such cases, the researchers also noted that females seem to have high higher levels of LH relative to their male counterparts. These studies conducted by the Zietchick Research Institute in collaboration with university scientists converge to suggest a critical role for LH in the eye and for vision.
Retinopathy of Prematurity (ROP)
Retinopathy of prematurity (ROP) is one of the primary causes of visual disability in children. ROP is indiscriminate in its affliction of premature babies; it affects infants of all races, ethnicities, and socioeconomic groups. Premature babies of very low birthweight (that is, less than 1,500 grams) are at the highest risk and approximately 60,000 babies in the USA alone are at risk of the development of ROP every single year. It is problematic that the currently available treatments are typically either laser surgery or drugs that need to be injected directly into the eye. These are expensive and invasive for patients and have several side effects associated with their use.
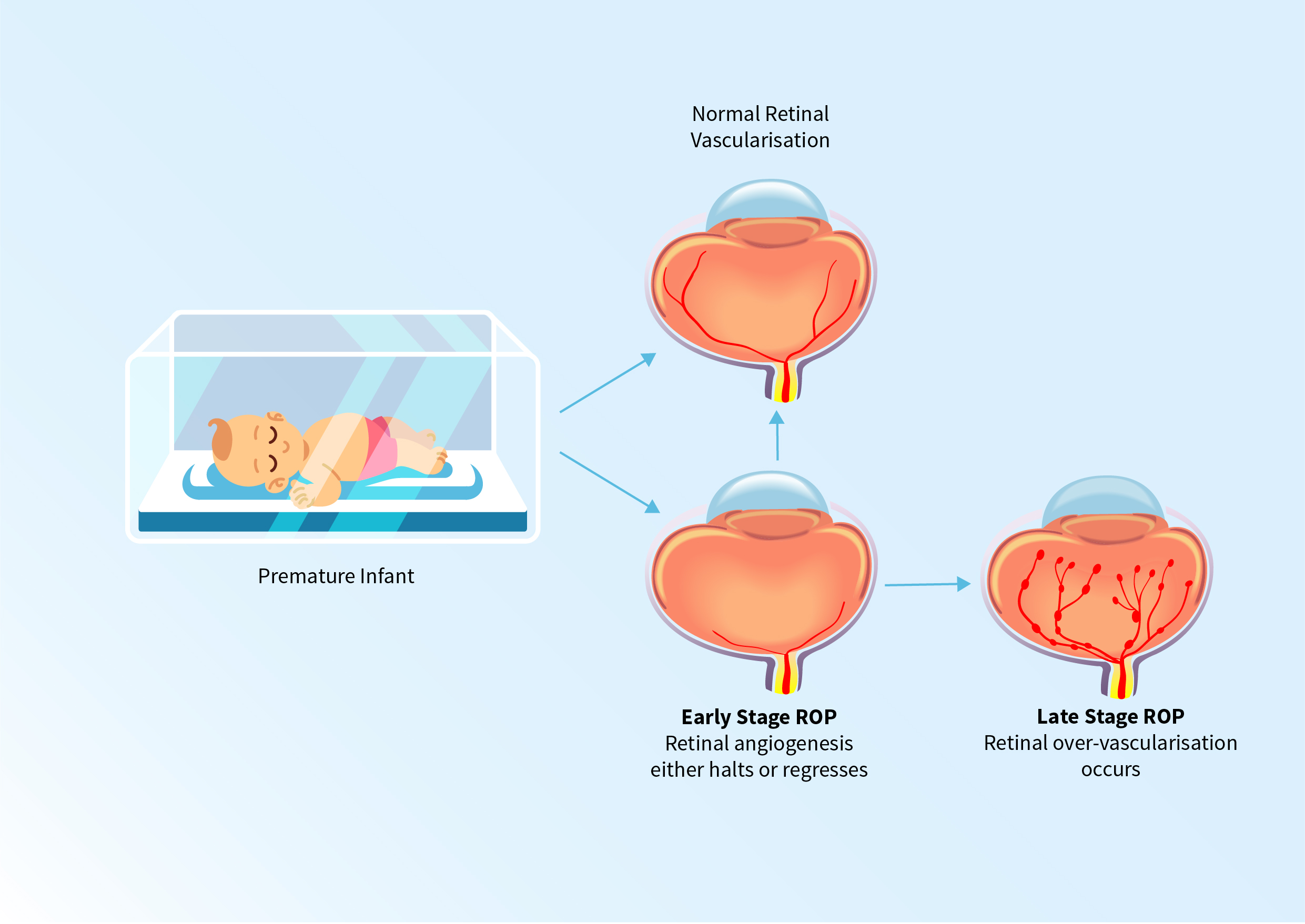
Stages of Retinopathy of Prematurity, Credit Zietchick Research Institute
Dr Movsas and her colleagues hope to dramatically change the horizon in terms of available treatments for ROP. They aim to develop a much-needed treatment that can be administered using eye drops. Not only would this provide a much simpler and less distressing intervention for young children, but such an approach would be more readily adopted in countries where eye surgeons are not as available as in the USA.
In a study published in 2018, Dr Movsas and colleagues investigated the contribution of gonadotropins to regulating levels of vascular endothelial growth factor (VEGF) in the developing eye. VEGF encourages the growth of new blood vessels. Premature infants are born before their eyes have fully developed, and sufficient levels of VEGF are needed for their retinal vessels to develop normally after birth. Low levels of this growth factor in the first weeks of life in babies are associated with early-stage ROP. In early-stage ROP, there is a halting of new blood vessel formation in the retina. Dr Movsas and her team found that young mouse eyes without gonadotropin receptors had lower levels of VEGF as well as a lower density of retinal blood vessels. Their work suggests a vital role for gonadotropins in the vascular maturation of the retina. This finding is now being used to support the development of novel strategies by the Zietchick Research Institute to prevent the onset of ROP.

Zietchick Research Institute is located in the Michigan Life Science and Innovation Center in Plymouth, MI
Gaining a Better Understanding
Since as far back as the 1940s, we have known that high oxygen levels used in the care of premature babies can cause ROP. For this very reason, as little oxygen as medically necessary is now administered. However, there are many other factors, in addition to oxygen, that also influence development of the eye. To better understand these factors, Dr Movsas and colleagues conducted a study of 113 babies who were born extremely prematurely and weighed less than 1,500 grams (under 3.3 lbs) at birth.
Often known as the ‘pregnancy hormone’, hCG helps promote the development of blood vessels in the uterus during pregnancy. Without adequate levels of hCG, pregnancy cannot be sustained by the mother, and low levels of the hormone are often used to diagnose miscarriage. Dr Movsas hypothesised that hCG also plays a key role in the development of blood vessels in the developing eye.
In premature babies, Dr Movsas and colleagues found that at 4 weeks old, blood levels of hCG are approximately the same as within the first days after birth. This suggests that premature babies make their own version of the pregnancy hormone – this was previously unknown. Moreover, they found that hCG levels tend to be lower in premature infants who develop ROP compared to those who do not, and that this is the case for both girls and boys. These findings have critical implications. This may be the first suggested role for hCG in human development, namely, its association with retinal vascularisation. Finally, given the presence of hCG receptors in other organs such as the gut and the brain, Dr Movsas points to the possibility that dysregulated hCG levels may be associated with other diseases associated with premature birth. Investigating this key hormone beyond vision may ultimately lead to improving the health of children who are born prematurely.

Dr Arivalagan Muthusamy, Chief Scientist of Zietchick
Research Institute (ZRI)
Onwards and Upwards
Having exciting evidence, thus far, for the potential involvement of gonadotropins in the development and maintenance of healthy vision, Dr Movsas and her colleagues now have an ambitious, evidence-based programme of research set in place. Dr Movsas explains, ‘Most vision scientists working in the field of vasoproliferative retinal disease concentrate on either diabetic retinopathy or retinopathy of prematurity. At the Zietchick Research Institute, we feel that we can best advance our understanding of these disorders by studying them both in conjunction.’
In addition to continuing her work on preventing blindness in premature infants, Dr Movsas aims to uncover the reasons why pregnancy presents such a significant risk factor for the worsening of diabetic retinopathy. Building upon her team’s findings to date, Dr Movsas predicts that hCG may increase VEGF in the maternal eye and this is what leads to the progression of diabetic eye disease during pregnancy. Dr Movsas proudly points out that the Zietchick Research Institute has undertaken the unique mission to develop therapeutics to optimise the eye health of both mothers and babies.
It is without a doubt that Dr Movsas and her colleagues have embraced a critically important challenge. By better understanding the underlying biological mechanisms of retinopathy in both mothers-to-be and premature babies, their research has the potential to transform the lives of many across the globe. By aiming to develop more readily accessible and even preventative treatments for conditions that eventually lead to blindness, the research undertaken by the Zietchick Research Institute provides a beacon of light in healthcare innovation worldwide.
Reference
https://doi.org/10.33548/SCIENTIA442
Meet the researcher

Dr Tammy Movsas, MD, MPH
Executive Director and Principal Investigator
Zietchick Research Institute, L3C
46701 Commerce Center Drive
Plymouth, MI
USA
Dr Tammy Movsas, Founder of Zietchick Research Institute (ZRI), has always had a passion for innovation and experimentation. Scientific ingenuity and constant questioning of assumptions have been an integral part of her life for as long as she can remember. Over the years, she has studied biochemistry, medicine, and epidemiology at some of world’s top universities: Harvard University (Cambridge, MA), Washington University School of Medicine (St Louis, MO), and University of Michigan School of Public Health (Ann Arbor, MI). She has completed a variety of residencies and fellowships at Washington National Eye Center (Washington DC), St Christopher’s Hospital for Children (Philadelphia, PA), Scheie Eye Institute, University of Pennsylvania (Philadelphia, PA), University of Michigan (Ann Arbor, MI), and Michigan State University (East Lansing, MI). She practiced clinical ophthalmology for 12 years before devoting her career to public health and research. Then, for six years, she served as Medical Director of the Midland County Department of Public Health in Midland, MI. During her tenure as Medical Director, Midland County’s health rankings rose each year reaching as high as #7 out of 83 Michigan counties. Filled with entrepreneurial spirit, Dr Movsas founded the Zietchick Research Institute in 2012. Within a short time, ZRI has become a world-class research organisation with a unique focus on developing therapeutics for maternal and child eye diseases. Dr Movsas has served as principal investigator on several National Institutes of Health and State-of-Michigan grants aimed to help advance our understanding of serious retinal eye disorders.
CONTACT
E: tmovsas@zietchick.com
FURTHER READING
TZ Movsas, N Paneth, IH Gewolb, Q Lu, G Cavey, A Muthusamy, The postnatal presence of human chorionic gonadotropin in preterm infants and its potential inverse association with retinopathy of prematurity, Pediatric Research, 2019, doi:10.1038/s41390-019-0580-8.
TZ Movsas, KY Wong, MD Ober, R Sigler, LM Lei, A Muthusamy, Confirmation of Luteinizing Hormone (LH) in Living Human Vitreous and the Effect of LH Receptor Reduction on Murine Electroretinogram, Neuroscience, 2018, 385, 1–10, doi: 10.1016/j.neuroscience.2018.05.049.
TZ Movsas, R Sigler, A Muthusamy, Elimination of Signaling by the Luteinizing Hormone Receptor Reduces Ocular VEGF and Retinal Vascularization during Mouse Eye Development, Current Eye Research, 2018, 43, 10, 1286–1289, doi: 10.1080/02713683.2018.1495740.

Creative Commons Licence
(CC BY 4.0)
This work is licensed under a Creative Commons Attribution 4.0 International License. 
What does this mean?
Share: You can copy and redistribute the material in any medium or format
Adapt: You can change, and build upon the material for any purpose, even commercially.
Credit: You must give appropriate credit, provide a link to the license, and indicate if changes were made.
More articles you may like
Grandmothers: Innovation Through Tradition
Grandmother Project – Change through Culture (GMP) is an organisation dedicated to documenting the role of grandmothers and demonstrating the effectiveness of grandmother-inclusive strategies in improving the health and well-being of women, children, and adolescents. GMP’s groundbreaking work challenges conventional wisdom to transform community-based interventions in Africa and beyond, harnessing a powerful but often overlooked resource: the wisdom and influence of grandmothers.
Dr Robert Larkin | Cultivating Change to Improve Soil Health and Increase Potato Yield
Environmental quality and food production are facing the pressing challenges of climate change and global population growth. Dr Robert Larkin from the United States Department of Agriculture-Agricultural Research Service (USDA-ARS) and a team of plant scientists developed and tested a range of crop management systems to help overcome these compounding challenges. Their work is improving soil health and increasing the yield of potato crops, contributing to the future food security of nations.
Professor Giorgio Buttazzo | Artificial Intelligence and a Crossroads for Humanity
Where do we stand with artificial intelligence? Might machines take over our jobs? Can machines become conscious? Might we be harmed by robots? What is the future of humanity? Professor Giorgio Buttazzo of Scuola Superiore Sant’Anna is an expert in artificial intelligence and neural networks. In a recent publication, he provides considered insights into some of the most pressing questions surrounding artificial intelligence and humanity.
Dr Ralf Adam | New Technologies Shaping the Future of Oral Hygiene
Understanding the efficiency of various toothbrush technologies is essential for achieving optimal oral health. Dr Ralf Adam, who leads a dedicated team at Procter & Gamble in Germany, is keen to investigate the complexities of these technologies. His team have provided new insights into the best toothbrush types for plaque removal and the maintenance of gum health. By highlighting the importance of informed oral care decisions and ongoing investigations, this vital research works towards ensuring everyone can achieve a brighter, healthier smile.




