Dr Dipak Panigrahy | Chemotherapy- and Carcinogen-induced Cell Debris Initiates Cancer Recurrence
Chemotherapy, one of the mainstays of cancer treatment, can unfortunately act as a double-edged sword. While achieving the intended aim of killing cancerous cells, it also generates an accumulation of cell debris, which in turn, promotes tumour growth by stimulating inflammation in the tumour microenvironment. Dr Dipak Panigrahy and his colleagues from Harvard Medical School, USA, have conducted several studies in mice showing that targeting the tumour cell debris-mediated surge of proinflammatory and protumourigenic factors provides a strategy for enhancing the efficacy of chemotherapy.
The Double-Edged Sword of Chemotherapy
With advances in genomics and drug discovery, chemotherapy is the frontline treatment for cancer now more than ever before. However, accumulating evidence from various animal models of the disease suggests that rather than simply killing the cancerous cells, chemotherapy can also initiate the recurrence of cancerous tumours. Unfortunately, the mechanisms behind this double-edged sword are still poorly understood. Working to resolve important questions about this critical issue is Dr Dipak Panigrahy, along with his colleagues at Harvard Medical School, USA.
Apoptosis is the process of programmed cell death, and this may trigger escape from tumour dormancy by causing a cellular stress response linked to inflammation. Dr Panigrahy and his colleagues argue that increased levels of spontaneous apoptotic cell death in the tumours of cancer patients are associated with poor prognosis in several cancer types.
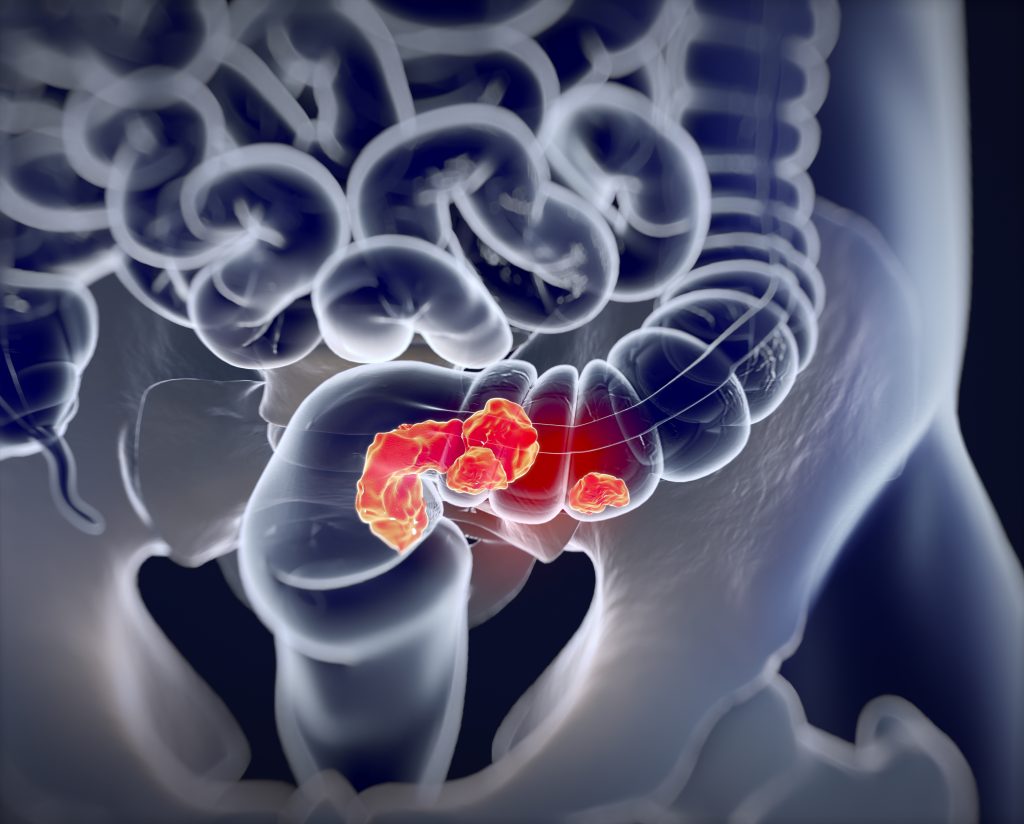
5-fluorouracil (5-FU) is a chemotherapeutic drug used to treat colorectal cancer. It reduces tumour mass by causing cell death, creating tumour cell debris in the form of apoptotic cells and cell fragments. Observing that apoptotic tumour cells can stimulate specialised cells known as macrophages and the production of proinflammatory cytokines, Dr Panigrahy and his colleagues proposed that 5-FU may be a source of tumour growth stimulation. In 2019, the Panigrahy laboratory published an important study that clearly demonstrated that 5-FU generates cellular debris that causes tumour cells and host macrophages to release a tumour factor known as osteopontin (OPN).
In clinical settings, OPN expression is linked to poor 5-year survival in many cancer types. OPN is a well-characterised factor that has been linked to cancer progression and angiogenesis, which is the growth of new blood vessels that tumours need to grow. Conventional chemotherapy may contribute to tumour progression and relapse via cell debris, suggesting that treating the tumour-promoting activity of cell debris is critical for the prevention of tumour recurrence.
In the 2019 study, Dr Panigrahy examined the cytotoxic activity of 5-FU in mice that were previously inoculated with colorectal cancer cells. As predicted, the researchers observed increased cell death in tumours that were treated with 5-FU compared with size-matched control tumours. Furthermore, the study confirmed that systemic 5-FU treatment and tumour cell debris increase OPN levels and that debris-stimulated tumour growth is mediated by enhanced tumour angiogenesis. The most important finding, however, was that pharmacologic and genetic ablation of OPN inhibited debris-stimulated tumour growth. Dr Panigrahy and his colleagues demonstrated that a combination of neutralising antibodies to inhibit OPN and continued treatment of 5-FU dramatically inhibited tumour growth.

Chemotherapy-generated Debris and Ovarian Cancer Resurgence
Epithelial ovarian cancer, a major cause of death in women worldwide, is characterised by a high tumour recurrence, which can occur in up to 70% of patients. To ascertain whether chemotherapy-generated debris is biologically relevant in ovarian cancer, via a similar mechanism initiated by 5-FU and mediated by OPN in colorectal cancer, Dr Panigrahy and his colleagues treated mouse and human cell lines with cytotoxic platinum- or taxane-based chemotherapeutic agents used for treating ovarian cancer. As a consequence of the treatment, the colleagues observed a surge of proinflammatory cytokines and bioactive lipid molecules known as eicosanoids, released by macrophages, in the tumour microenvironment. The findings of this study were published in 2019 in the prestigious journal, the Proceedings of the National Academy of Sciences (PNAS).
The research team also observed that the presence of debris alone without macrophages in the culture medium resulted in minimal to undetectable levels of cytokines, confirming that the release of lipid mediators and cytokines is macrophage-dependent. The PNAS study showed that the combined pharmacological inhibition of the cyclooxygenase-2 (COX-2) and soluble epoxide hydrolase (sEH) pathways prevented the surge of both cytokines and lipid mediators by macrophages. These results confirmed that ovarian cancer patients may benefit from the suppression of eicosanoid and cytokine mediators, protecting the body from a therapy-induced debris-mediated cytotoxic and tumourigenic response.
Aspirin-triggered Mediators as Optimal Chemopreventive Agents
Many studies suggest that the nonsteroidal anti-inflammatory drug (NSAID) aspirin is potent in counteracting the formation of tumours. Despite numerous reports confirming its beneficial properties in cancer prevention, the biochemical mechanisms behind this unique antitumour activity of aspirin compared with other NSAIDs remain poorly understood. Cyclooxygenase (COX)-1 and COX-2 are key targets of aspirin and are involved in the biosynthesis of proinflammatory lipids, such as prostaglandins. Dr Panigrahy and his colleagues published another study in 2019 showing that aspirin not only blocks the biosynthesis of prostaglandins, but also stimulates the endogenous production of anti-inflammatory mediators termed ‘aspirin-triggered specialised pro-resolving mediators’ (AT-SPMs), such as ‘aspirin-triggered resolvins’ (AT-RvDs) and ‘aspirin-triggered lipoxins’ (AT-LXs).
The research team demonstrated that treatment of mice with AT-RvDs or AT-LXs inhibited primary tumour growth by enhancing macrophage removal of tumour cell debris and inhibiting the production of macrophage-secreted proinflammatory cytokines. Following the publication of the 2019 study, AT-SPMs, including resolvins, have been considered in clinical studies for their tumour-preventing activity. Dr Panigrahy and his colleagues have shown that, given the risks associated with chronic low-dose aspirin intake, mediators such as aspirin-triggered resolvins and other AT-SPMs may be a more desirable therapeutic option, since they display more potent antitumour activity and are devoid of aspirin-related toxicity.
Resolvins Enhance Cancer Therapy by Clearing Cell Debris
As demonstrated in many studies by the Panigrahy team, dead and dying tumour cells greatly affect the tumour microenvironment. This leaves the medical profession with a dilemma between treating tumours with chemotherapy and minimising the effects of debris-induced tumour progression. Resolving this dilemma is paramount to preventing tumour recurrence after therapy.
In a study published in 2017, Dr Panigrahy and his colleagues demonstrated that apoptotic debris stimulates tumour growth through the action of phosphatidylserine (PS), a modified amino acid that is present on the surface of apoptotic cells. The study showed that blocking PS in the debris with a recombinant protein or an anti-PS neutralising antibody significantly inhibited debris-stimulated tumour growth in a dose-dependent manner.
The 2017 study adds further evidence in support of using specialised pro-resolving mediators, such as resolvins, to clear apoptotic debris. The novel approach alongside chemotherapy would greatly prevent tumour recurrence and enhance the benefits of cancer therapy. The observations were supported by the results of a 2019 study in which Dr Panigrahy and his colleagues demonstrated that the resolution of inflammation via resolvins, before surgery, inhibited the formation of new tumour growth, inducing robust anticancer T cell immunity in mice affected by Lewis lung carcinoma.
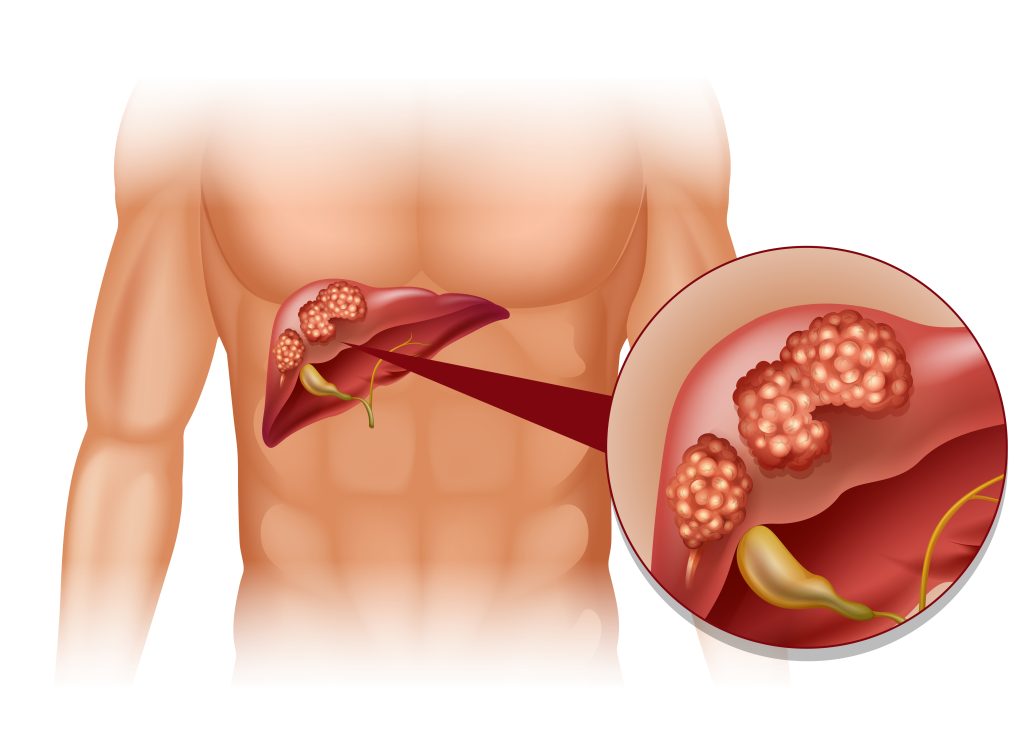
Resolution of Inflammation Halts Liver Cancer Progression
Building on the observations published in previous years, Dr Panigrahy and his colleagues recently published a new study on the effects of inflammation on the changes to the tumour microenvironment triggered by cytokine and eicosanoid storms during hepatocellular carcinoma (HCC). Aflatoxin B1 (AFB1), a mycotoxin produced by Aspergillus fungi, may play a causative role in 4.6 to 28.2% of all HCC cases worldwide. Aflatoxin-induced HCC is most prevalent in developing countries due to the regular consumption of food contaminated with aflatoxins.
HCC is associated with excessive production of proinflammatory cytokines, including TNF-α and IL-6, which lead to apoptotic cell death in multiple cell types. AFB1 can also negatively impact macrophages by impairing their ability to remove cell debris. By causing excessive production of oxidative stress, proinflammatory cytokines start a cascade that leads to DNA damage and new tumour growth, correlating with poor patient survival. Dr Panigrahy and his colleagues demonstrated that tumour cells killed by AFB1 stimulate primary HCC growth when co-injected in mice with a nontumourigenic inoculum of tumour cells and that the malignant growth is dependent on a macrophage-derived eicosanoid and cytokine storm that also involves mediators that promote the formation of new blood vessels.
Dr Panigrahy and colleagues demonstrated that dual COX-2/sEH inhibitors can be administered during and immediately after periods of high exposure to aflatoxins, resulting in a physiological switch from a pattern of inflammation to the resolution of inflammation. By targeting the debris-mediated eicosanoid and cytokine storm, via clearance of tumour cell debris, dual COX-2/sEH inhibition may provide an effective strategy for the prevention of AFB1-induced hepatocellular carcinoma.
SHARE
DOWNLOAD E-BOOK
LISTEN TO THE AUDIO
REFERENCE
https://doi.org/10.33548/SCIENTIA842
MEET THE RESEARCHER

Dr Dipak Panigrahy
Harvard Medical School
Harvard University
Boston, MA
USA
Dr Dipak Panigrahy obtained his MD in 1994 from Boston University School of Medicine, Boston, MA. During his postdoctoral studies, Dr Panigrahy specialised in Vascular Biology and Surgery and is now Assistant Professor of Pathology at Harvard Medical School. The Panigrahy Laboratory studies a class of lipid autacoid mediators known as eicosanoids and their pathophysiologic roles in the development of cancer. This translates into an ongoing collaboration with industry to study eicosanoid modulating drugs in experimental cancer models. As an outstanding clinician-scientist, Dr Panigrahy has written numerous publications on cancer treatment, has chaired numerous international conferences and symposia on cancer biology, and sat on the editorial boards of several prestigious scientific journals.
CONTACT
W: https://www.bidmc.org/research/research-by-department/pathology/laboratories/dipak-panigrahy-lab
Professor Charles Serhan
Harvard Medical School
Harvard School of Dental Medicine
Harvard University
Boston, MA
USA
Professor Charles Serhan completed his PhD at the New York University School of Medicine in 1982. Following postdoctoral research positions in Sweden and London, he joined the faculty at Harvard Medical School in 1987. Professor Serhan is currently the Simon Gelman Professor of Anaesthesia (Biochemistry and Molecular Pharmacology) at Harvard Medical School and Professor of Oral Medicine, Infection and Immunity at Harvard School of Dental Medicine. He is also Director of the Center for Experimental Therapeutics and Reperfusion Injury at Brigham and Women’s Hospital.
CONTACT
W: https://serhanlab.bwh.harvard.edu/
Professor Bruce Hammock
University of California, Davis
Davis, CA
USA
Professor Bruce Hammock completed his PhD at the University of California, Davis, in 1973. He is now the Distinguished Professor of Entomology in the College of Agricultural and Environmental Sciences at the same institution. He is a Founding Member of the University of California Davis Comprehensive Cancer Center, as well as a member of the National Academy of Science and Academy of Inventors.
CONTACT
W: https://www.biopestlab.ucdavis.edu/
FUNDING
DP is supported by the generous support of Credit Unions Kids at Heart Team and the C.J. Buckley Pediatric Brain Tumor Fund (DP).
FURTHER READING
J Deng, H Yang, VW Haak, et al., Eicosanoid regulation of debris-stimulated metastasis, Proceedings of the National Academy of Sciences, 2021, 118(41), e2107771118. DOI: https://doi.org/10.1073/pnas.2107771118
A Fishbein, W Wang, H Yang, et al., Resolution of eicosanoid/cytokine storm prevents carcinogen and inflammation-initiated hepatocellular cancer progression, Proceedings of the National Academy of Sciences, 2020, 117(35), 21576–21587. DOI: https://doi.org/10.1073/pnas.2007412117
J Chang, S Bhasin, D Bielenberg, et al., Chemotherapy-generated cell debris stimulates colon carcinoma tumor growth via osteopontin, The FASEB Journal, 2019, 33(1), 114–125. DOI: https://doi.org/10.1096/fj.201800019RR
A Gartung, J Yang, V Sukhatme, et al., Suppression of chemotherapy-induced cytokine/lipid mediator surge and ovarian cancer by a dual COX-2/sEH inhibitor, Proceedings of the National Academy of Sciences, 2019, 116(5), 1698–1703. DOI: https://doi.org/10.1073/pnas.1803999116
M Gilligan, A Gartung, M Sulciner, et al., Aspirin-triggered proresolving mediators stimulate resolution in cancer, Proceedings of the National Academy of Sciences, 2019, 116(13), 6292–6297. DOI: https://doi.org/10.1073/pnas.1804000116
D Panigrahy, A Gartung, J Yang, et al., Preoperative stimulation of resolution and inflammation blockade eradicates micrometastases, The Journal of Clinical Investigation, 2019, 129(7), 2964–2979. DOI: https://doi.org/10.1172/JCI127282
M Sulciner, C Serhan, M Gilligan, et al., Resolvins suppress tumor growth and enhance cancer therapy, Journal of Experimental Medicine, 2017, 215(1), 115–140. DOI: https://doi.org/10.1084/jem.20170681

REPUBLISH OUR ARTICLES
We encourage all formats of sharing and republishing of our articles. Whether you want to host on your website, publication or blog, we welcome this. Find out more
Creative Commons Licence (CC BY 4.0)
This work is licensed under a Creative Commons Attribution 4.0 International License. 
What does this mean?
Share: You can copy and redistribute the material in any medium or format
Adapt: You can change, and build upon the material for any purpose, even commercially.
Credit: You must give appropriate credit, provide a link to the license, and indicate if changes were made.
SUBSCRIBE NOW
Follow Us
MORE ARTICLES YOU MAY LIKE
Dr Ralf Adam | New Technologies Shaping the Future of Oral Hygiene
Understanding the efficiency of various toothbrush technologies is essential for achieving optimal oral health. Dr Ralf Adam, who leads a dedicated team at Procter & Gamble in Germany, is keen to investigate the complexities of these technologies. His team have provided new insights into the best toothbrush types for plaque removal and the maintenance of gum health. By highlighting the importance of informed oral care decisions and ongoing investigations, this vital research works towards ensuring everyone can achieve a brighter, healthier smile.
Dr Toby Phesse | Revealing the Mysteries of Wnt Signalling: Novel Approaches to Beating Cancer
Cancer remains a leading cause of mortality worldwide, and the need for new, more effective treatments remains an urgent challenge. Dr Toby Phesse from Cardiff University in the UK focuses on the role of the Wnt receptor found on the surface of cells and its involvement with cell communication and cancer growth, bringing fresh hopes for new therapeutic options.
Dr Vijay Reddy | The Virus World Database: An Invaluable Resource for Public Health and Healthcare
Severe viral disease presents an ongoing challenge to the health of humankind. While unparalleled developments in science and technology are improving our understanding of such viruses, this information needs to be readily accessible to researchers to ensure continued progress in public health and healthcare. Dr Vijay Reddy and his colleagues at the Hormel Institute (University of Minnesota) developed the Virus World database, an invaluable resource that details the genome, structure, and host of practically every discovered virus to date.
Professor Ralf Herwig | Deciphering the Enigma of Vitamin D and the Immune System
Vitamin D has been studied as a treatment for a large number of diseases and conditions, from cancer to autism to COVID-19. However, its mode of action is not completely understood. Professor Ralf Herwig carries out his research at HG Pharma GmbH (Austria) and Ulster University (UK). His vital work explores the role of vitamin D in the body with a view to unlocking its potential as a treatment for a variety of health conditions involving the immune system.