Dr Richard Hayes – Bringing an End to the HIV Epidemic Through Universal Testing and Treatment
Worldwide, an estimated 38 million people are living with HIV. Many are still unaware of their status and so are not linked to care and treatment which can prevent them from passing HIV onto their partners and infants and keep them healthy. Dr Richard Hayes from the London School of Hygiene and Tropical Medicine in the UK has led the HIV Prevention Trials Network’s 071 (PopART) trial over the past ten years. This dedicated international collaboration of experts has successfully demonstrated how universal testing and treatment can reduce new HIV infections in Zambia, South Africa and beyond.
HIV/AIDS and Effective Treatment
HIV is a viral infection transmitted through unprotected sex. It can also be passed on from a mother to child through giving birth and breastfeeding, as well as through sharing needles with an HIV-positive person.
HIV infects cells of the immune system. Without treatment with antiretroviral therapy (ART), HIV ultimately causes severe immune damage leading to life-threatening infections and cancers. However, life-saving ART has now dramatically transformed survival for people living with HIV and limits the virus in their bodies to levels below which HIV cannot be passed on to sexual partners or infants.
However, the only way to ensure all people living with HIV start ART and remain healthy while also reducing the risk of passing their infection to their partners and infants is to know their HIV status. This requires regular and accurate HIV testing amongst all sexually active populations. When an individual receives a positive HIV result, it is recommended that they start taking ART. This combination of drugs blocks HIV replication, preventing further damage to the immune system.

Credit: Kim Cloete.
Working Together to End the HIV/AIDS Epidemic
Although new HIV infections have gradually decreased over the last 10 years, it remains a major global health issue, with around 38 million people living with HIV worldwide – 1.7 million of whom are children below 14 years. Since the beginning of the epidemic in the 1980s, over 30 million people have lost their lives to AIDS-related causes.
Among the worst impacted are those living in Eastern and Southern Africa, where almost 21 million people live with HIV (more than half of all HIV cases globally). With the aim of ending the AIDS epidemic, in 2014 the Joint United Nations Programme on HIV/AIDS (UNAIDS) set the 90-90-90 targets – that is, for 90% of people with HIV to know their HIV status, for 90% of those diagnosed to receive sustained ART and for 90% of people on ART to show viral suppression by 2020. Going forward from 2020 to 2030, these targets are now set even higher at 95-95-95.
As part of working towards these ambitious goals, the HIV Prevention Trials Network (HPTN) conducted the HPTN 071 (PopART) trial, a collaborative study into universal testing and treatment for HIV. This study was led by Dr Richard Hayes from the London School of Hygiene and Tropical Medicine along with Dr Sarah Fidler at Imperial College, Dr Helen Ayles at the Zambia AIDS Related Tuberculosis Project (Zambia) and Dr Nulda Beyers and Dr Peter Bock at the Desmond Tutu TB Centre at Stellenbosch University in South Africa. Multitudes of organisations across several countries and research disciplines were also involved in this effort to find a solution to the global health issue of HIV. From local health centres in Zambia and South Africa to huge USA funding agencies and academic institutions in the UK, a truly collaborative effort was initiated.

Credit: Kim Cloete.
‘We found that this universal testing and treatment approach could be delivered effectively at community level, and over three years it reached the UNAIDS targets for knowledge of HIV status, ART coverage and HIV viral suppression.’
Universal Testing and Treatment
An important strategy proposed to reduce new HIV infections is the application of universal testing and treatment. According to Dr Hayes, ‘The idea is simple: that everyone in the community should be offered a regular HIV test so that all community members know their HIV status. And that all those who are diagnosed HIV-positive should be linked to care and encouraged to start ART immediately.’ If a high enough proportion of HIV-positive people are aware of their status and are treated with ART to become virally suppressed, new infections among a given community should be significantly reduced.
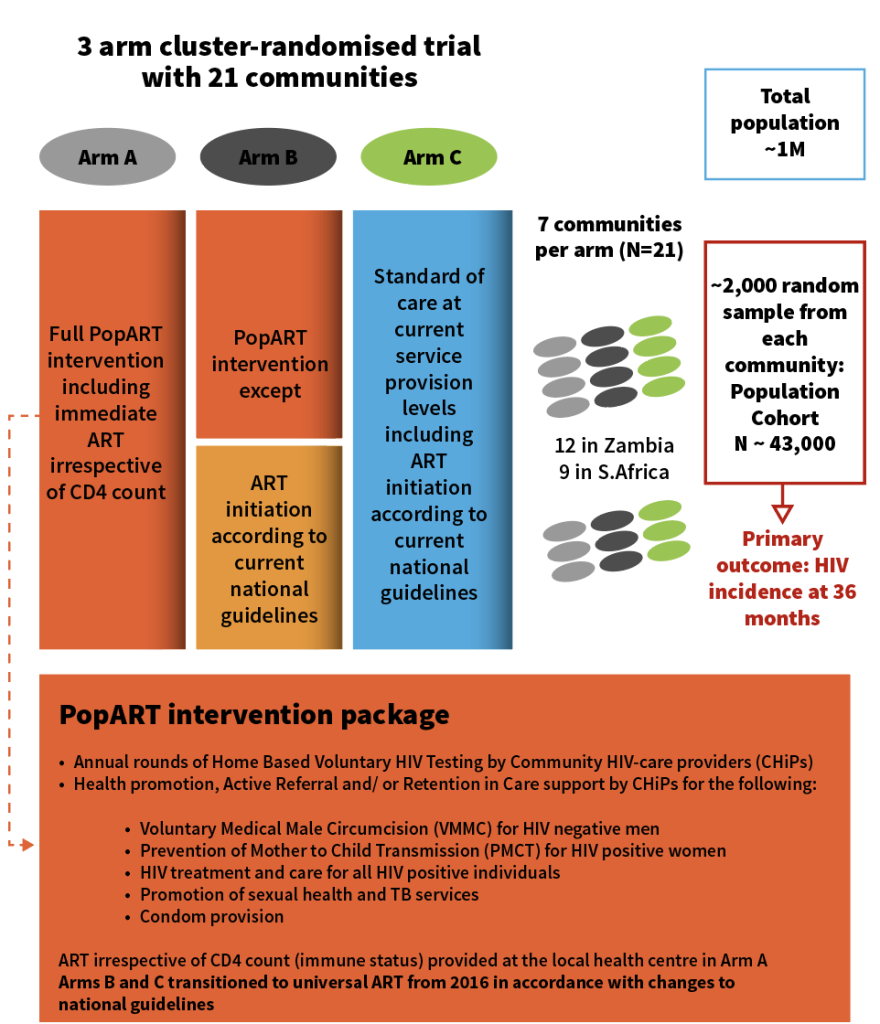
The PopART trial tested whether the strategy of universal testing and treatment would be possible in low-income settings and if so, whether it would have an impact on reducing new HIV infections. A total of 21 communities in South Africa and Zambia with around 50,000 residents and an overall HIV prevalence of around 15% were chosen to take part. Each community was assigned to one of the three arms of the study.
In Arm A, annual, voluntary HIV testing was provided by community health workers who went directly to the doors of everyone in the community. Those who tested positive were linked to care for immediate, free ART at their local health centre. Those who tested negative were directed to different proven HIV prevention measures such as condoms and voluntary male circumcision. In Arm B, communities followed the same strategy, but HIV treatment was given according to respective national guidelines. Here, some guidelines specified ART could only be started once the immune cells reached a certain threshold of damage. Finally, Arm C acted as a control and these communities received HIV testing and prevention services according to their local standard of care and treatment according to national guidelines.
At four time points over the course of the study (which ran from 2013 to 2018), members of the study team visited a random group of participants who lived in the PopART communities and who had given their consent to contribute to the trial outcome measures. At each visit, these participants provided questionnaire data and completed a blood test for HIV infection. The HIV results of the blood tests from these study participants informed the researchers about the impact of the different community approaches in each of the study arms on HIV incidence.
The Impact of PopART
Critically, the researchers found that utilising the universal testing and treatment strategy allowed them to meet the UNAIDS 90-90-90 targets, meaning the intervention presented a feasible method at the community level. By the end of the study, their interventions had reduced the overall rate of new HIV infections in the communities by 20%. Even more impressively, Dr Hayes describes how, ‘mathematical models fitted to the data from our trial estimated that if the intervention were to be kept in place over a longer time period, the impact would increase over time, eventually reaching a reduction of around 50%.’
However, the team did notice that certain groups were more difficult to find and engage in the intervention. More specifically, younger people aged between 15 and 24 years, and especially young men, had the lowest ART coverage by the end of the study. This important finding led the researchers to recommend that special efforts should be made in future work to reach these groups to ensure better coverage and uptake of the intervention.
Having confirmed that universal testing and treatment can reduce the number of new HIV infections in Zambia and South Africa when delivered to large urban and peri-urban communities, the researchers wanted to know how much money this intervention costs. An economic evaluation of the findings determined that the PopART home-based intervention package cost between $5.10–$6.80 in Zambia and between $6.40–$8.20 in South Africa per person per year. This was deemed to be cost-effective in the long term if sustained.
Overall, findings were strongly in support of the use of door-to-door universal testing and treatment, suggesting this is a feasible and community-accepted intervention. Many people were appreciative that they did not have to wait in queues for testing and did not have to face judgement from their community through being able to take the tests in the privacy of their own homes. Clearly, broad coverage and high uptake can be achieved if the whole community is reached and interventions are sustained. When this happens, the team proposes that new HIV cases will continue to drop.
The PopART study team concluded that ‘…this universal testing and treatment approach could be delivered effectively at community level, and over three years it reached the UNAIDS targets for knowledge of HIV status, ART coverage and HIV viral suppression, and significantly reduced the number of new HIV infections.’
This dedicated work by the study team has made vital strides forward in improving the quality of life and longevity of life for people living with HIV. If these approaches are implemented on a wider scale, we could be much closer to finally bringing an end to the devastating HIV epidemic.
SHARE
DOWNLOAD E-BOOK
LISTEN TO THE AUDIO
REFERENCE
https://doi.org/10.33548/SCIENTIA813
MEET THE RESEARCHERS

The HIV Prevention Trials Network HPTN 071 (PopART) Trial
Principal Investigator: Dr Richard Hayes
Department of Infectious Disease Epidemiology
London School of Hygiene and Tropical Medicine
London
UK

Dr Helen Ayles

Dr Sarah Fidler
Established in 2000, the HIV Prevention Trials Network (HPTN) is a worldwide clinical trials collaboration bringing together investigators, ethicists, members of the community and other partners to develop and test the safety and efficacy of interventions designed to prevent the transmission of HIV. The HPTN 071 (PopART) trial was led by Dr Richard Hayes at the London School of Hygiene and Tropical Medicine (UK) in collaboration with Dr Sarah Fidler at Imperial College (also in the UK), Dr Helen Ayles at the Zambia AIDS Related Tuberculosis Project (Zambia) and finally, Dr Nulda Beyers and Dr Peter Bock at the Desmond Tutu TB Centre at Stellenbosch University in South Africa.
CONTACT
W: https://www.hptn.org/; https://www.lshtm.ac.uk/aboutus/people/hayes.richard
FUNDING
National Institute of Allergy and Infectious Diseases
U.S. President’s Emergency Plan for AIDS Relief
International Initiative for Impact Evaluation
Bill & Melinda Gates Foundation
National Institute on Drug Abuse
National Institute of Mental Health
FURTHER READING
RJ Hayes, D Donnell, S Floyd, et al., Effect of Universal Testing and Treatment on HIV Incidence — HPTN 071 (PopART), New England Journal of Medicine, 2019, 381(3), 207–218. DOI: https://doi.org/10.1056/NEJMoa1814556R
Thomas, WJM Probert, R Sauter, et al., Cost and cost-effectiveness of a universal HIV testing and treatment intervention in Zambia and South Africa: evidence and projections from the HPTN 071 (PopART) trial, The Lancet Global Health, 2021, 9(5), 668–680. DOI: https://doi.org/10.1016/S2214-109X(21)00034-6
S Floyd, K Shanaube, B Yang, et al., HIV testing and treatment coverage achieved after 4 years across 14 urban and peri-urban communities in Zambia and South Africa: An analysis of findings from the HPTN 071 (PopART) trial, PLoS Medicine, 2020, 17(4), 1003067. DOI: https://doi.org/10.1371/journal.pmed.1003067


REPUBLISH OUR ARTICLES
We encourage all formats of sharing and republishing of our articles. Whether you want to host on your website, publication or blog, we welcome this. Find out more
Creative Commons Licence (CC BY 4.0)
This work is licensed under a Creative Commons Attribution 4.0 International License. 
What does this mean?
Share: You can copy and redistribute the material in any medium or format
Adapt: You can change, and build upon the material for any purpose, even commercially.
Credit: You must give appropriate credit, provide a link to the license, and indicate if changes were made.
SUBSCRIBE NOW
Follow Us
MORE ARTICLES YOU MAY LIKE
Dr Ralf Adam | New Technologies Shaping the Future of Oral Hygiene
Understanding the efficiency of various toothbrush technologies is essential for achieving optimal oral health. Dr Ralf Adam, who leads a dedicated team at Procter & Gamble in Germany, is keen to investigate the complexities of these technologies. His team have provided new insights into the best toothbrush types for plaque removal and the maintenance of gum health. By highlighting the importance of informed oral care decisions and ongoing investigations, this vital research works towards ensuring everyone can achieve a brighter, healthier smile.
Dr Toby Phesse | Revealing the Mysteries of Wnt Signalling: Novel Approaches to Beating Cancer
Cancer remains a leading cause of mortality worldwide, and the need for new, more effective treatments remains an urgent challenge. Dr Toby Phesse from Cardiff University in the UK focuses on the role of the Wnt receptor found on the surface of cells and its involvement with cell communication and cancer growth, bringing fresh hopes for new therapeutic options.
Dr Vijay Reddy | The Virus World Database: An Invaluable Resource for Public Health and Healthcare
Severe viral disease presents an ongoing challenge to the health of humankind. While unparalleled developments in science and technology are improving our understanding of such viruses, this information needs to be readily accessible to researchers to ensure continued progress in public health and healthcare. Dr Vijay Reddy and his colleagues at the Hormel Institute (University of Minnesota) developed the Virus World database, an invaluable resource that details the genome, structure, and host of practically every discovered virus to date.
Professor Ralf Herwig | Deciphering the Enigma of Vitamin D and the Immune System
Vitamin D has been studied as a treatment for a large number of diseases and conditions, from cancer to autism to COVID-19. However, its mode of action is not completely understood. Professor Ralf Herwig carries out his research at HG Pharma GmbH (Austria) and Ulster University (UK). His vital work explores the role of vitamin D in the body with a view to unlocking its potential as a treatment for a variety of health conditions involving the immune system.