Dr Tanja Jovanovic – Trauma in Childhood: How Adversity Affects Brain Development
Exposure to childhood trauma increases the risk of developing mental health issues in adulthood. However, the processes through which this occurs are currently unknown. Using magnetic resonance imaging, laboratory-based measurements of fear, and the assessment of clinical symptomatology, Dr Tanja Jovanovic from Wayne State University is investigating the effect that trauma has on brain development. She hopes her findings will help identify those children at risk of anxiety or post-traumatic stress disorder so that preventative measures can be put in place to ensure brighter futures for children in their adulthood years.
Post-traumatic Stress Disorder
Around one in four adults will face mental health issues during their lifetime. Depression, anxiety and post-traumatic stress disorder (PTSD) are all prevalent, with about 8% of the population experiencing the latter. PTSD can develop after traumatic events, ranging from experiencing violence to witnessing a car accident. The resultant symptoms in adults can be numerous, such as vivid and distressing re-experiencing of the trauma, struggling to fall and stay asleep, strong physical reactions to reminders or triggers, panic attacks and irritability. For some, these symptoms last for a few weeks, for others, it can be much longer. PTSD is also associated with high levels of comorbidity with other forms of psychopathology such as depression, anxiety and alcohol/drug abuse.
Children with PTSD similarly present with symptoms of sleep problems and aggression. However, they can also exhibit developmentally related behaviours, such as reproducing their trauma through play or drawings, forgetting previously mastered skills such as toilet training, and demonstrating separation anxiety.
Critically, adversity at a young age can alter how a child’s brain develops and this may lead to mental health issues such as PTSD, anxiety and depression later in life. But how this happens is not yet known.
Dr Tanja Jovanovic is a Professor in the Department of Psychiatry and Behavioural Neurosciences at Wayne State University in Detroit. She and her team are working on unravelling the science behind how trauma exposure can lead to PTSD, so that they can predict who may be most at risk to later psychopathology. Importantly, if approaches aiming to prevent the development of psychopathology can be implemented with children who have been deemed high-risk thanks to Dr Jovanovic’s research, they may be spared from future psychological distress.
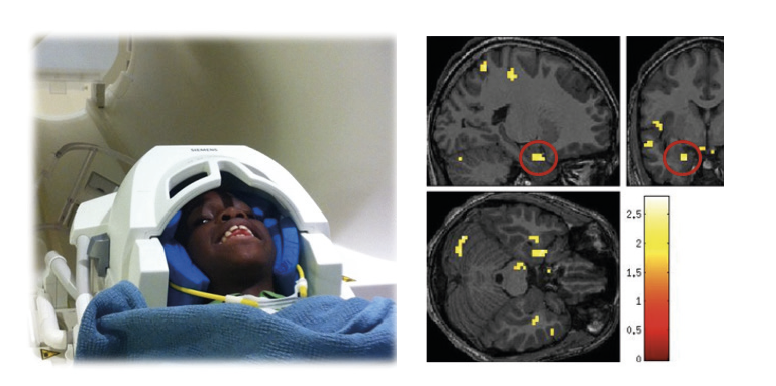
Testing brain responses to fear in the laboratory. Credit Tanja Jovanovic.
Influences on the Response to Trauma in Childhood
Throughout the years, Dr Jovanovic has published many studies on psychopathology in children. With colleagues, she has established that girls and boys react differently to trauma, with girls more likely to blame themselves and fear a repeat of the ordeal. Such differences in how individuals react to trauma lead to differential risks for the development of subsequent mental health problems.
Age differences also occur in relation to the experience of trauma. A study published by Dr Jovanovic and colleagues in 2016 showed that the availability of a mother during a fear conditioning experiment (involving the learning of fear in response to a given stimulus) in younger children, but not adolescents, allowed them to better discriminate between dangerous and safe signals. This effect is known as ‘maternal buffering’ and is consistent with the perspective that a child’s parenting environment is significant for their learning of danger and safety signals. However, the quality of the mother-child relationship, at least as rated by the mother, did not influence the maternal buffering effect. In another study, they found that children of mothers who had experienced a lot of trauma and had many PTSD symptoms also had problems learning safety signals, independent of their age and own traumatic experiences.
Another way a mother can impact their child’s mental health is through their level of emotionality. If a mother is less able to manage her emotions (known as emotion dysregulation) and finds parenting to be very stressful and overwhelming, she is more likely to pass on anxiety to her children, which puts them at higher risk for additional mental health issues.
Testing the Impact of Trauma on Brain Development in the Laboratory
Dr Jovanovic and her team are currently conducting a longitudinal study to investigate the effect of trauma on brain development and how this might lead to PTSD. Longitudinal studies are used to observe the same variables (or outcomes) over a period of time. In this case, the critical variable is how trauma affects a child’s brain development. During this ongoing study, children in Detroit aged 9 years, along with their primary caregivers, are being recruited to participate for over 3 years. When they first start the study, they are asked if they have experienced any traumatic events in their lives, complete some laboratory tests, and undergo a magnetic resonance imaging (MRI) brain scan.
An MRI forms detailed images using radio waves and a magnetic field. Because this technique allows clinicians to see irregularities in tissues and organs, it is often used to identify tumours, strokes and other disorders. Dr Jovanovic is using MRI to see how different parts of children’s brains are physically altered as a result of trauma.
Functional magnetic resonance imaging (fMRI) is slightly different from MRI because it is used to show brain activity. When a part of the brain is active, it requires more oxygen to function, so oxygenated blood flow increases to that area. An fMRI detects these changes and, for Dr Jovanovic, allows her to see which parts of the brain are being used in children with varying levels of fear.
The laboratory tests the team perform to measure fear are known as fear conditioning paradigms, such as the fear-potentiated startle (FPS) test. This involves measuring the reflexive (involuntary) physiological reaction to a neutral stimulus such as a loud sound or bright light, for example. The neutral stimulus is repeatedly paired with an aversive air blast until it starts to signal danger, while a different, unpaired, stimulus signals safety. The individual’s responses to these stimuli are recorded physiologically, such as through the eyeblink contraction and heart rate. Reacting more strongly than normal to the danger or safety stimulus may reveal an anxiety or trauma-related disorder, or a higher ongoing level of fear.
Every 6 months, the participants return to the laboratory and are asked if they have experienced any new trauma, and each year they undergo another fMRI brain scan.

Trauma’s Mark on the Brain
Although data collection is still in the early stages, a number of interesting findings have already emerged. Despite the observation that the children recruited have experienced significant violence within their neighbourhood, they are resilient, with little evidence of PTSD symptomatology. This seems to be due to higher activation in their regulatory and protective brain areas such as the hippocampus and prefrontal cortex when the fear areas, like the amygdala, are also activated. Regulatory and protective areas in the brain are in charge of controlling functions like emotion, reasoning and judgement. Dr Jovanovic says that this, ‘may suggest that children with high trauma have higher levels of fear, but also that other areas are working harder to control the fear.’ She also notes that ‘As we continue to follow these children as they grow it will be important to see which children continue to be resilient and which start to show symptoms so that we can learn how to help them.’
Not only were the activation levels of parts of the participants’ brains altered but so were the sizes. More specifically, exposure to urban violence resulted in a smaller hippocampus and larger amygdala. While these structural changes may have the potential to lead to future psychopathology, they could also provide a survival mechanism to allow the brain to adapt to the threats in the environment and overcome the trauma.
Previous studies have shown that having a specific version of a gene called ADCYAP1R1 is associated with increased FPS and PTSD in adult women. However, Dr Jovanovic wanted to examine how this genotype (the version of the gene) and trauma affects development in children as well. Her work indicated that there is a link between higher fear in children with greater exposure to violence and this variation of ADCYAP1R1. They found that this fear worsens with age, so they think children with this genotype may be at higher risk of PTSD as they get older. Gender was also an important factor, as girls with this variation of the gene showed more fear than boys. In addition, they found that girls who have experienced trauma show accelerated pubertal development, which leads to higher fear responses.
‘As part of our research, we have uncovered several biological factors that can make some children more vulnerable to PTSD and anxiety.’
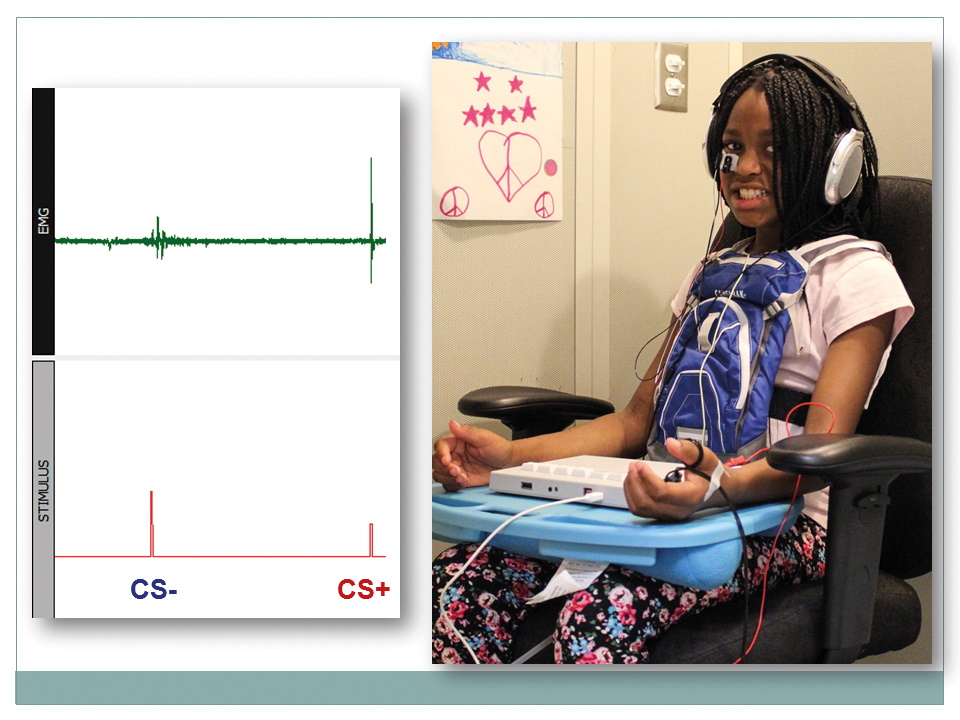
Measuring electromyography in response to presented stimuli in the laboratory. Credit Tanja Jovanovic.
Next Steps
Dr Jovanovic is planning further studies into psychopathology in relation to genetics and neurobiology. Hormonal changes, sex differences and the environment will also be explored to discover how they affect brain development and fear. She hopes that her research will be used to identify those who are most likely to develop future mental health issues as a result of experiencing trauma.
In her own words, Dr Jovanovic explains, ‘our research has indicated several areas that interventions can target for vulnerable children to prevent future psychological distress.’ PTSD can have a long-lasting effect, not just on the sufferer, but also their loves ones. Marital problems are more common with people who have PTSD and their children are more likely to have anxiety, depression and behavioural problems. But, if at-risk children are identified, they can be helped through interventions such as counselling, exercise, mindfulness and many other methods, to allow them to lead happier lives with brighter futures.
Reference
https://doi.org/10.33548/SCIENTIA641
Meet the researcher

Dr Tanja Jovanovic
Department of Psychiatry and Behavioural Neurosciences
Wayne State University
Detroit, MI
USA
Dr Tanja Jovanovic received her PhD in Neuroscience and Animal Behaviour from Emory University in Atlanta, Georgia. Afterwards, she served as Assistant Professor in the Department of Psychiatry and Behavioral Sciences at the Emory University School of Medicine. She is now a Professor in the Department of Psychiatry and Behavioural Neurosciences and the David and Patricia Barron Chair for PTSD Neurobiology at Wayne State University. Dr Jovanovic directs the Detroit Trauma Project which investigates how urban trauma exposure impacts the brain. In addition, she is the lead investigator on several federally funded grants from the National Institutes of Health. Her many achievements include over 170 published papers, serving on national and international grant review panels and an Independent Investigator Award from the Brain and Behavior Research Foundation.
CONTACT
E: tjovanovic@med.wayne.edu
W: https://psychiatry.med.wayne.edu/profile/gr5613
Twitter: @TJovanovic_PhD; Lab: @DTP_Wayne
KeEY COLLABORATORS
Dr Anais Stenson, Wayne State University
Dr Seth Norrholm, Wayne State University
Dr Hilary Marusak, Wayne State University
Dr Arash Javanbakhtm, Wayne State University
Dr Jennifer Stevens, Emory
Dr Sanne van Rooij, Emory
Dr Kerry Ressler, Harvard University
Dr Nicole Nugent, Brown University
Dr Nim Tottenham, Columbia University
Dr Tracy Bale, University of Maryland
FUNDING
National Institute of Mental Health
Brain and Behavior Research Foundation (NARSAD)
FURTHER READING
G Hartzell, AF Stenson, SJH van Rooij, et al., Intergenerational effects of maternal PTSD: Roles of parenting stress and child sex, Psychological Trauma, 2020, doi:10.1037/tra0000542.
AF Stenson, SJH van Rooij, SE Carter, et al., A legacy of fear: Physiological evidence for intergenerational effects of trauma exposure on fear and safety signal learning among African Americans, Behavioural Brain Research, 2020, 113017, doi:10.1016/j.bbr.2020.113017.
AF Stenson, NR Nugent, SJH van Rooij, et al., Puberty drives fear learning during adolescence, Developmental Science, 2020, 00:e13000, doi:10.1111/desc.13000.
SJH van Rooij, RD Smith, AF Stenson, et al., Increased activation of the fear neurocircuitry in children exposed to violence, Depression and Anxiety, 2020, 37, 303–312, doi:10.1002/da.22994.
M Cao, A Powers, D Cross, et al., Maternal emotion dysregulation, parenting stress, and child physiological anxiety during dark-enhanced startle, Developmental Psychobiology, 2017, 59, 1021–1030.
SJH van Rooij, D Cross, JS Stevens, et al., Maternal buffering of fear-potentiated startle in children and adolescents with trauma exposure, Social Neuroscience, 2017, 12, 22–31.
K Gamwell, M Nylocks, D Cross, et al., Fear Conditioned Responses and PTSD Symptoms in Children: Sex Differences in Fear-Related Symptoms, Developmental Psychobiology, 2015, 57, 799–808.

Want to republish our articles?
We encourage all formats of sharing and republishing of our articles. Whether you want to host on your website, publication or blog, we welcome this. Find out more
Creative Commons Licence
(CC BY 4.0)
This work is licensed under a Creative Commons Attribution 4.0 International License. 
What does this mean?
Share: You can copy and redistribute the material in any medium or format
Adapt: You can change, and build upon the material for any purpose, even commercially.
Credit: You must give appropriate credit, provide a link to the license, and indicate if changes were made.
More articles you may like
Grandmothers: Innovation Through Tradition
Grandmother Project – Change through Culture (GMP) is an organisation dedicated to documenting the role of grandmothers and demonstrating the effectiveness of grandmother-inclusive strategies in improving the health and well-being of women, children, and adolescents. GMP’s groundbreaking work challenges conventional wisdom to transform community-based interventions in Africa and beyond, harnessing a powerful but often overlooked resource: the wisdom and influence of grandmothers.
Dr Robert Larkin | Cultivating Change to Improve Soil Health and Increase Potato Yield
Environmental quality and food production are facing the pressing challenges of climate change and global population growth. Dr Robert Larkin from the United States Department of Agriculture-Agricultural Research Service (USDA-ARS) and a team of plant scientists developed and tested a range of crop management systems to help overcome these compounding challenges. Their work is improving soil health and increasing the yield of potato crops, contributing to the future food security of nations.
Professor Giorgio Buttazzo | Artificial Intelligence and a Crossroads for Humanity
Where do we stand with artificial intelligence? Might machines take over our jobs? Can machines become conscious? Might we be harmed by robots? What is the future of humanity? Professor Giorgio Buttazzo of Scuola Superiore Sant’Anna is an expert in artificial intelligence and neural networks. In a recent publication, he provides considered insights into some of the most pressing questions surrounding artificial intelligence and humanity.
Dr Ralf Adam | New Technologies Shaping the Future of Oral Hygiene
Understanding the efficiency of various toothbrush technologies is essential for achieving optimal oral health. Dr Ralf Adam, who leads a dedicated team at Procter & Gamble in Germany, is keen to investigate the complexities of these technologies. His team have provided new insights into the best toothbrush types for plaque removal and the maintenance of gum health. By highlighting the importance of informed oral care decisions and ongoing investigations, this vital research works towards ensuring everyone can achieve a brighter, healthier smile.




