Dr Thomas Shaffer – Dr Tariq Rahman | Innovative New Technology to Monitor Children’s Breathing
Monitoring a patient’s breathing closely is vital to medical care. However, it comes with a whole set of challenges in young children and those with certain medical conditions. Dr Thomas Shaffer and Dr Tariq Rahman from the Nemours Children’s Hospital, Delaware, USA, work together to develop novel technologies to address this issue and drive better outcomes for their younger patients.
Take a Deep Breath
Pulmonary function testing (PFT) provides clinicians with critical information about the patient’s respiratory physiology. Many currently available PFT methods can take time to carry out and require cooperation from the patient, which can be difficult in younger children. Respiratory inductive plethysmography (RIP) is a technique used to monitor a patient’s breathing patterns. It is noninvasive, can be completed in 5 to 10 minutes, and requires minimal cooperation from the patient. RIP works by measuring the change in volume in the abdomen and ribcage using bands placed around the chest and tummy. This can then be used to give work of breathing (WOB) indices related to the amount of energy expended to take a breath.
Dr Thomas Shaffer and Dr Tariq Rahman from the Department of Biomedical Research, Nemours Children’s Hospital, Delaware, USA, have developed a new technology that allows continuous, real-time monitoring using RIP. They aim to introduce their technology to assist with PFT in a number of medical conditions and situations in which it can prove challenging.
Monitoring the Youngest of Patients
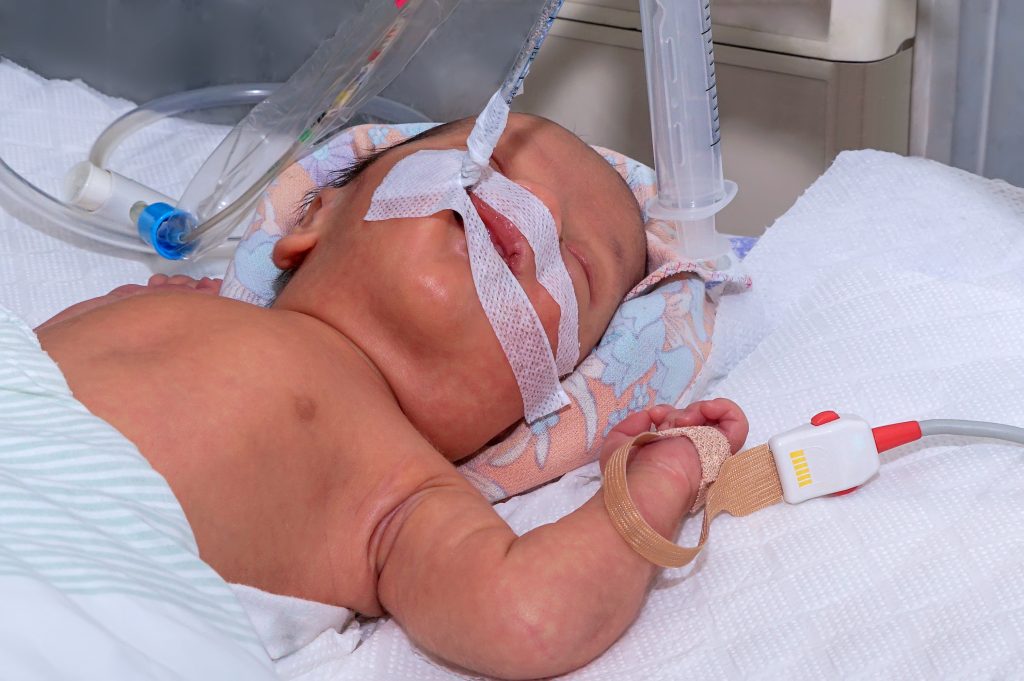
Premature babies are at risk of a condition called bronchopulmonary dysplasia (BPD). It commonly occurs in babies born at under 30 weeks or with a birth weight of under 1 kg, usually because these babies need extra help breathing and end up being supported by a ventilator for several weeks. One way in which BPD can be prevented is to use noninvasive respiratory support, such as a high-flow nasal cannula (HFNC), which basically pushes oxygen out of a small tube into the nose and, in turn, the lungs. Although using HFNC is better tolerated by the baby and inflicts less damage to the airway and lung tissue, it may not be as effective as the ventilation methods.
Dr Shaffer and his colleagues looked into how feasible it was to use RIP to monitor breathing, specifically WOB indices, and adjust the flow of oxygen on the HFNC accordingly in real time. Their aim was to enable the doctors to optimise the amount of support provided by the HFNC by allowing them to respond directly to the individual baby’s needs. The team closely monitored 21 babies using this method, and 62% showed an improvement in their breathing – a 20% improvement in their WOB indices. They also showed improvements in their oxygen saturation (the amount of oxygen in the blood), and their breathing was more stable.
Dr Shaffer and his team also successfully used RIP to monitor very small premature babies as part of a study looking into kangaroo mother care, where the infant has prolonged skin-to-skin contact with the mother. This helps calm the tiny baby and improves their chances of survival.

Kangaroo care (skin-to-skin contact).
The pneuRIPTM
Dr Shaffer joined forces with Dr Rahman to develop the pneuRIPTM, a more user-friendly, high-tech, less bulky version of the traditional RIP. Their device uses a novel wireless analyser that serves up real-time measures of WOB data, displaying it all on an iPad.
A game changer for the team, they next decided to test the feasibility of the pneuRIPTM in different sets of patients. They assessed their newly developed RIP system in an outpatient clinic setting in children with neuromuscular diseases. These diseases tend to worsen over time and need continuous monitoring, with some patients eventually going into respiratory failure requiring long-term ventilation support.
Many of the current methods available to assess breathing in these types of diseases are time-consuming, expensive, and very tiring for the patient. Being able to offer alternative methods of breathing assessments, as well as being able to do these at the patient’s home, would undoubtedly allow better management and levels of care.
Dr Shaffer and Dr Rahman studied 43 participants aged between 5 and 18 years old. In total, 22 patients had a neuromuscular disease, and 21 were healthy children. They were able to successfully use the pneuRIPTM on all the children, and the device provided instant pulmonary function test data. The children showed patterns of breathing and WOB indices as expected for their condition, compared to the healthy children.
Tackling Rare Diseases
Duchenne muscular dystrophy (DMD) is a rare, progressive condition that is diagnosed in childhood. It is caused by a faulty gene and results in the muscles weakening over time. Eventually, it affects the heart and lungs, so pulmonary function testing is regularly required. Morquio syndrome is another rare genetic condition which affects multiple organ systems, including the respiratory system, due to a problem metabolising certain types of sugars. Respiratory failure is the leading cause of death in these patients.
Dr Shaffer and Dr Rahman reviewed the feasibility of using the pneuRIPTM for both of these patient groups. They reported 100% compliance in the studies they conducted for both patients with Morquio syndrome and DMD. Their RIP system was found to be accurate, easy to administer, and portable, making it suitable to use in a variety of patient care settings, such as at home, in clinics, and in the emergency department.

The pneuRIPTM. Credit Thomas Shaffer
Improving Machine Learning with pneuRIPTM
Thoracoabdominal asynchrony (TAA) is a mismatch in how the rib cage and abdomen move whilst breathing. Its presence can point to several different lung diseases, such as obstructive sleep apnoea, asthma, respiratory distress and chronic obstructive pulmonary disease. Dr Shaffer and Dr Rahman used their RIP device to gather data about TAA, which was then used to teach a computer how to recognise it on readings from other patients.
They reported that their system offered an accurate automated approach (Machine Learning) to identify TAA that reduced the time to get a diagnosis. Their approach was able to identify TAA in patients with neuromuscular diseases with an accuracy of 90.3%. The team say that such an automated system could be very useful for monitoring and assessing patients with respiratory conditions. They were also able to offer improved methods for better machine-learning performance, which included a comprehensive graphical display of the changes in lung function over time.
Helping Children with Severe Cerebral Palsy
With such high compliance rates and a plethora of positive results with the pneuRIPTM technology, Dr Shaffer and Dr Rahman will now test it out on patients with cerebral palsy (CP). CP is a group of conditions of varying severity that affect the movement and coordination caused by a problem in the brain around the time of birth. A third of CP patients have severe symptoms, often resulting in weakening of the respiratory muscles and progressive lung disease, which increases the risk of fatal pneumonia.
The researchers plan to use their technology to monitor for respiratory problems such as TAA and obstructive sleep apnoea, with the aim of detecting potential problems before they turn into severe complications. They would also like to investigate the relationship between TAA measures and the degree of scoliosis in CP patients who use a wheelchair. Scoliosis is the sideway curve of the backbone, which, in this group of patients, is thought to impact the muscles of the ribcage, in turn affecting breathing.

Credit Thomas Shaffer.
Easing Chronic Pain with Yoga
In addition to working with CP patients, Dr Shaffer and Dr Rahman aim to help children with chronic pain. They argue that yoga, as a complementary therapy, can help children with chronic pain and emotional distress better cope with their symptoms. It also helps to improve lung function and can be used in conjunction with biofeedback to help patients connect their cognitive and physical processes. During biofeedback, noninvasive sensors are used to measure physiological signals such as heart rate and breathing rate, which are then displayed to the patient during yoga therapy. The patient can then learn to use the same calming techniques in the absence of biofeedback.
Dr Shaffer and Dr Rahman want to use the pneuRIPTM to show the beneficial effect of posture (or asana) and pranayama (or breathing) in the use of yoga for chronic pain. They are creating a biofeedback mobile application with a user-friendly interface to allow visualisation of the respiratory process in order to improve the effectiveness of breathing training. They also aim to incorporate haptic feedback that can guide breathing. These are subtle touch-like gestures such as a small vibration from a smartwatch or similar device. The colleagues plan on incorporating the Apple Watch with their technology, as it can offer haptic feedback, and it also has several sensors, allowing additional health data, like heart rate and blood oxygen levels, to be recorded. In addition to developing the biofeedback mobile app, the researchers also aim to use their device to measure the immediate and cumulative impact of yoga on breathing in patients with chronic pain by recording data from multiple yoga sessions.
The pneuRIPTM technology offers many advantages over the currently available methods of pulmonary function testing. This innovative device, along with the development of a mobile app, has the potential to significantly improve the care and management of very sick children around the world.
SHARE
DOWNLOAD E-BOOK
REFERENCE
https://doi.org/10.33548/SCIENTIA964
MEET THE RESEARCHERS

Dr Thomas H. Shaffer
Department of Biomedical Research and Center for Pediatric Lung Research
Nemours Children’s Hospital
Wilmington, DE
USA
Dr Thomas Shaffer obtained his PhD from Drexel University in Philadelphia. He completed a postdoctoral fellowship at the University of Pennsylvania School of Medicine, where he was later promoted to Assistant Professor of Physiology and Medicine. He has also held the position of Associate Professor at the Temple University School of Medicine. Currently, Dr Shaffer is Professor Emeritus of Physiology and Paediatrics, Professor of Paediatrics at Thomas Jefferson Medical College, and the Director of the Centre for Paediatric Research at Nemours Children’s Health. He is also the Director of the Centre for Paediatric Lung Research, and Associate Director for Biomedical Research, Delaware Valley. During his prestigious career spanning four decades, he has received many awards and grants, and he is the holder of 34 patents. His expertise in pulmonary research is particularly dedicated to the needs of the neonatal and paediatric populations.
CONTACT
E: thomas.shaffer@nemours.org
W: http://centerforpediatricresearch.org

Dr Tariq Rahman
Department of Biomedical Research
Nemours Children’s Hospital
Wilmington, DE
USA
Dr Tariq Rahman obtained his PhD in Mechanical Engineering from Drexel University, Philadelphia, and later became a postdoctoral fellow at the Alfred I. duPont Hospital for Children in Wilmington, DE. He currently holds the position of Principal Research Engineer and Director of the Centre for Orthopaedics Research and Development (CORD) at Nemours Children’s Hospital. Dr Rahman specialises in rehabilitation and biomedical engineering, specifically focusing on tremor reduction, robotics, orthotics, orthopaedics, and pulmonology. As an esteemed academic, he has published over 75 papers and has been funded by the Department of Education, National Institutes of Health, Cure SMA, and The Swank Foundation.
CONTACT
E: trahman@nemours.org
W: https://www.bio.udel.edu/people/trahman
KEY COLLABORATORS
Nemours Children’s Hospital, Wilmington, DE
Abigail Strang, MD
Robert Heinle, MD
Aaron Chidekel, MD
Jobayer Hosain, PhD
Shunji Tomatsu, MD, PhD
Madhavi Ratnagiri, PhD
Yosef Levenbrown, DO
Katie Salamon, PhD
Wade Shrader, MD
Christiana Care, Newark, DE
Kelley Kovatis, MD
Robert Locke, DO
Amy Mackley, MSN
Creative Micro Designs, Newark, DE
Ralph Page, BS
Adam Page, PhD
FUNDING
National Institutes of Health: P20RR020173; P20GM103464; P30GM114736; 1R21HD111958-01; 1R41AT012155-01; 1R21EB032025-01; 1R01HD102545-01A1
Center for Advanced Technology (CAT)
FURTHER READING
KZ Kovatis, RG Locke, AB Mackley, et al., Adjustment of high flow nasal cannula rates using real-time work of breathing indices in premature infants with respiratory insufficiency, Journal of Perinatology, 2021, 41, 1711–1717. DOI: https://doi.org/10.1038/s41372-021-00977-z
MV Ratnagiri, L Ryan, A Strang, et al., Machine learning for automatic identification of thoracoabdominal asynchrony in children, Pediatric Research, 2021, 89, 1232–1238. DOI: https://doi.org/10.1038/s41390-020-1032-1
L Ryan, T Rahman, A Strang, et al., Diagnostic differences in respiratory breathing patterns and work of breathing indices in children with Duchenne muscular dystrophy, PLoS ONE, 2020, 15(1), e0226980, https://doi.org/10.1371/journal.pone.0226980
A Strang, L Ryan, T Rahman, et al., Measures of respiratory inductance plethysmography (RIP) in children with neuromuscular disease, Pediatric Pulmonology, 2018, 59(3), 1260–1268. DOI: https://doi.org/10.1002/ppul.24134

REPUBLISH OUR ARTICLES
We encourage all formats of sharing and republishing of our articles. Whether you want to host on your website, publication or blog, we welcome this. Find out more
Creative Commons Licence (CC BY 4.0)
This work is licensed under a Creative Commons Attribution 4.0 International License. 
What does this mean?
Share: You can copy and redistribute the material in any medium or format
Adapt: You can change, and build upon the material for any purpose, even commercially.
Credit: You must give appropriate credit, provide a link to the license, and indicate if changes were made.
SUBSCRIBE NOW
Follow Us
MORE ARTICLES YOU MAY LIKE
Dr Ralf Adam | New Technologies Shaping the Future of Oral Hygiene
Understanding the efficiency of various toothbrush technologies is essential for achieving optimal oral health. Dr Ralf Adam, who leads a dedicated team at Procter & Gamble in Germany, is keen to investigate the complexities of these technologies. His team have provided new insights into the best toothbrush types for plaque removal and the maintenance of gum health. By highlighting the importance of informed oral care decisions and ongoing investigations, this vital research works towards ensuring everyone can achieve a brighter, healthier smile.
Dr Toby Phesse | Revealing the Mysteries of Wnt Signalling: Novel Approaches to Beating Cancer
Cancer remains a leading cause of mortality worldwide, and the need for new, more effective treatments remains an urgent challenge. Dr Toby Phesse from Cardiff University in the UK focuses on the role of the Wnt receptor found on the surface of cells and its involvement with cell communication and cancer growth, bringing fresh hopes for new therapeutic options.
Dr Vijay Reddy | The Virus World Database: An Invaluable Resource for Public Health and Healthcare
Severe viral disease presents an ongoing challenge to the health of humankind. While unparalleled developments in science and technology are improving our understanding of such viruses, this information needs to be readily accessible to researchers to ensure continued progress in public health and healthcare. Dr Vijay Reddy and his colleagues at the Hormel Institute (University of Minnesota) developed the Virus World database, an invaluable resource that details the genome, structure, and host of practically every discovered virus to date.
Professor Ralf Herwig | Deciphering the Enigma of Vitamin D and the Immune System
Vitamin D has been studied as a treatment for a large number of diseases and conditions, from cancer to autism to COVID-19. However, its mode of action is not completely understood. Professor Ralf Herwig carries out his research at HG Pharma GmbH (Austria) and Ulster University (UK). His vital work explores the role of vitamin D in the body with a view to unlocking its potential as a treatment for a variety of health conditions involving the immune system.